What Is Leg Discoloration?
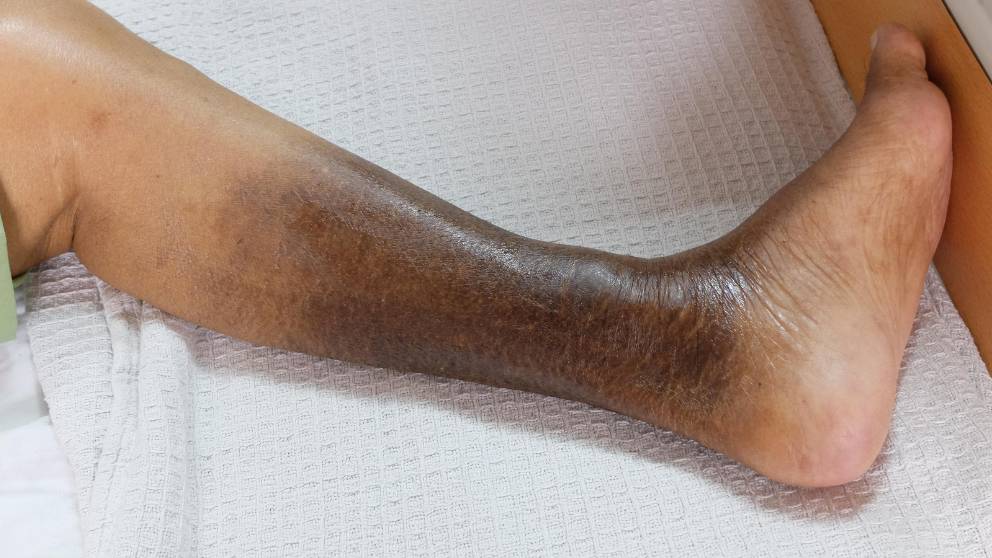
Leg discoloration, often called venous stasis dermatitis, occurs when the skin color on the feet or lower legs changes due to underlying circulatory problems. This condition happens when the veins in your legs have difficulty returning blood to your heart, causing blood to pool in the legs. Over time, this increased pressure leads to fluid and blood cells leaking into the surrounding tissues, resulting in swelling, inflammation, and skin discoloration.
The discoloration can range from a light reddish-brown to a dark purple and is commonly associated with chronic venous insufficiency (CVI) or deep vein thrombosis (DVT). Individuals with compromised circulation, whether due to lifestyle factors or underlying medical conditions, are more prone to this problem. If untreated, leg discoloration can worsen and lead to more severe health issues like skin ulcers and infections, which are more challenging to manage.
Understanding the causes, risk factors, and signs of leg discoloration is vital for managing this condition effectively and improving your overall quality of life.
When Should I See a Doctor for Leg Discoloration?
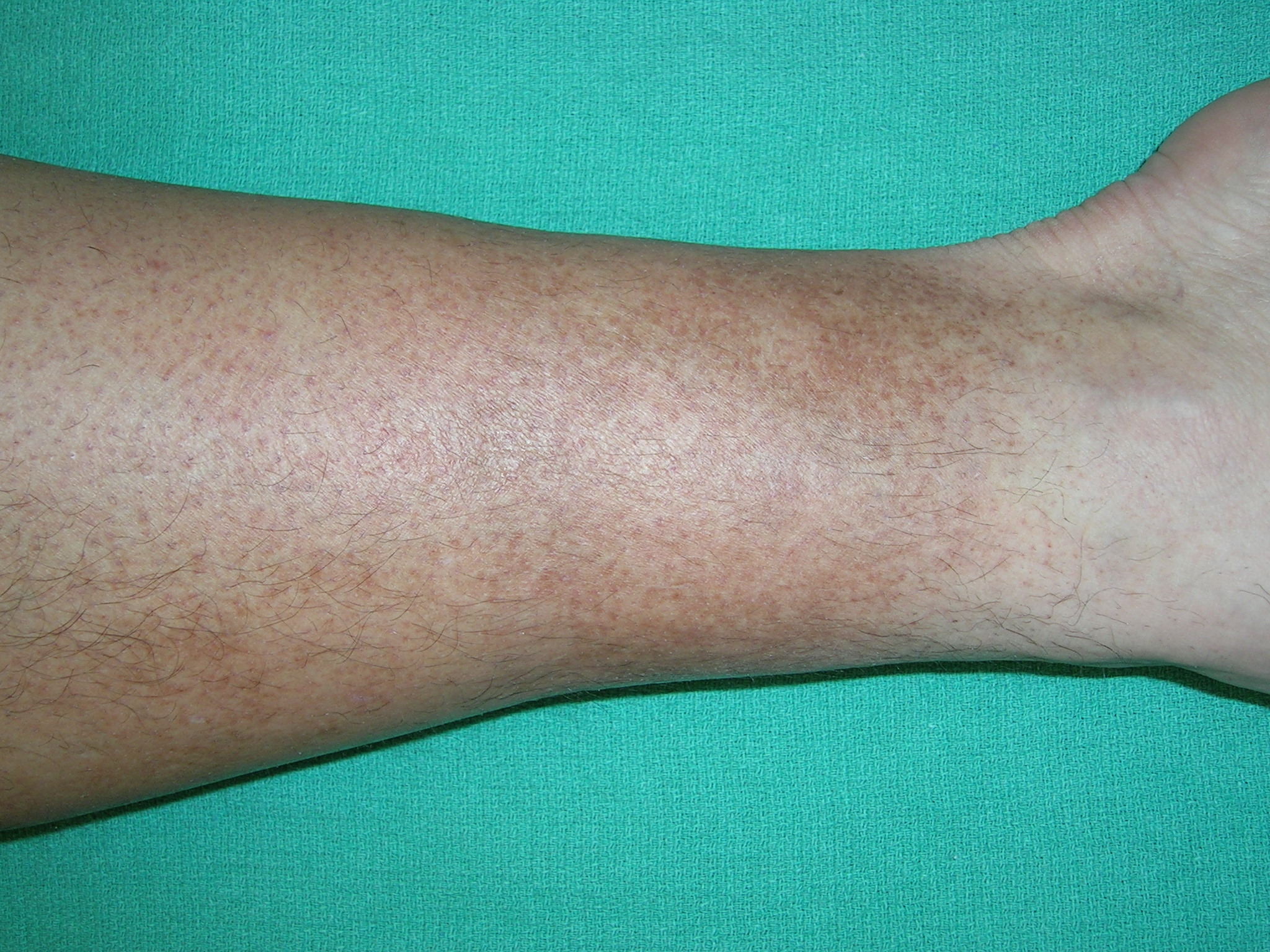
Suppose you notice any changes in the color of your skin around your legs, particularly if the discoloration is accompanied by swelling, pain, or other symptoms. In that case, it’s essential to consult a doctor. While leg discoloration can start as a mild cosmetic issue, it may indicate more severe vascular conditions such as chronic venous insufficiency or blood clots.
You should see a healthcare provider if you experience:
- Persistent swelling in your legs
- Darkening or reddening of the skin, especially near the ankles
- Itchy or scaly skin
- Pain or discomfort in the lower legs
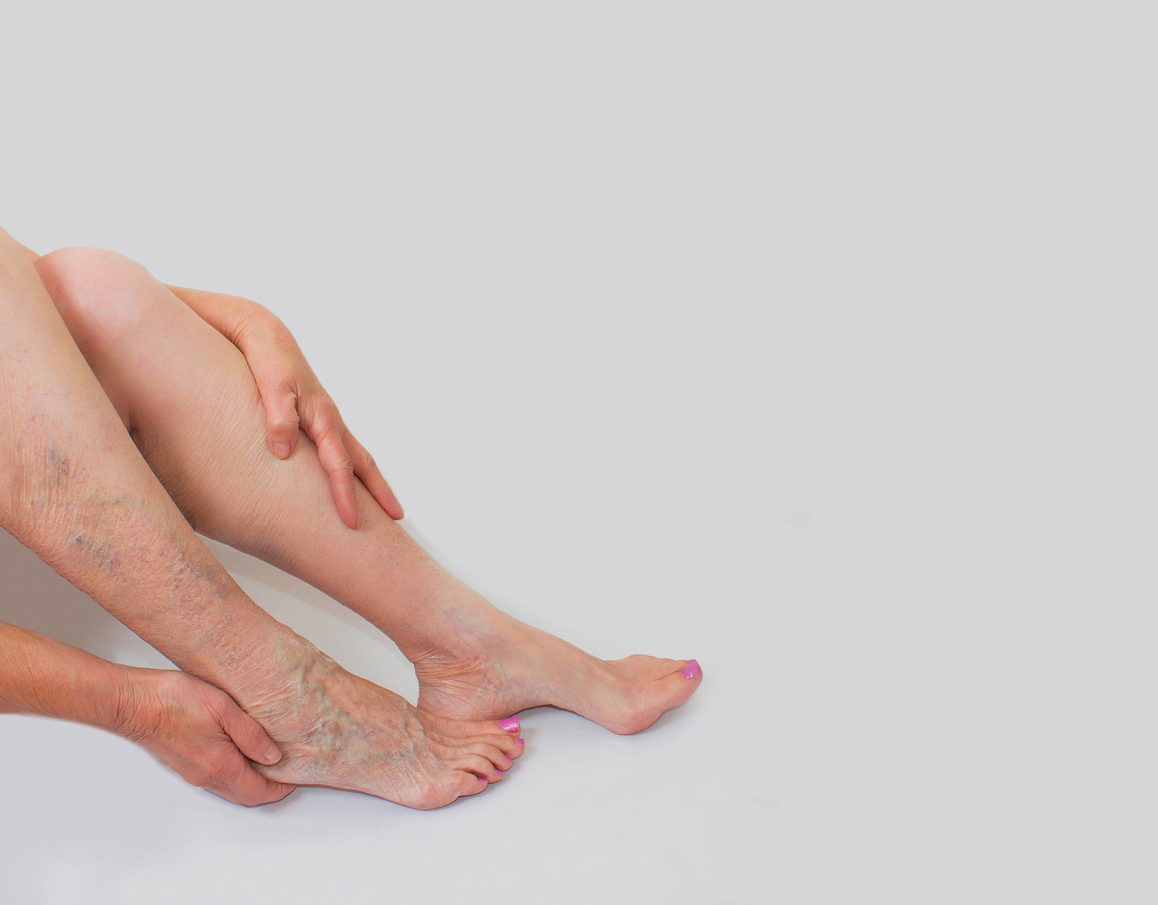
- Signs of varicose veins or spider veins
Early medical intervention can prevent further damage and help manage the symptoms before they become more severe. Your primary care provider may refer you to a vascular specialist to evaluate the underlying causes and recommend treatment options.
What Causes Leg Discoloration?
Leg discoloration is commonly caused by venous insufficiency, a condition where the veins fail to function properly, leading to blood pooling in the legs. Several factors contribute to the development of leg discoloration, including:
Age
As we age, the veins in our legs can lose their elasticity, weakening the one-way valves that keep blood flowing back to the heart. This can result in blood pooling and subsequent discoloration.
Weight
Carrying excess weight places additional pressure on the veins in your legs, making it harder for the blood to flow efficiently. Over time, this increased pressure can lead to venous insufficiency and discoloration.
Immobility
Sitting or standing for long periods can significantly impair circulation. Without movement, the calf muscles cannot help pump blood back to the heart, leading to increased venous pressure and leg discoloration.
Varicose Veins
Varicose veins are more than just a cosmetic issue; they indicate that the veins are not functioning as they should, which can cause discoloration due to blood pooling in the legs.
Blood Clots (DVT)
Blood clots in the deep veins can block proper blood flow, causing swelling and discoloration. This is a serious condition that requires immediate medical attention.
Pregnancy
The additional weight and hormonal changes during pregnancy can weaken the vein walls, leading to blood pooling and discoloration in the legs.
Heart and Kidney Conditions
Issues with the heart or kidneys can also lead to poor circulation, which can cause leg discoloration because blood and fluids are not adequately circulated.
What are Non-Vascular Causes of Leg Discoloration?
Leg discoloration can result from various non-vascular conditions involving skin, metabolic, or inflammatory factors. Bruising from trauma often causes red or purple marks that change color as they heal. Post-inflammatory hyperpigmentation, seen after eczema, psoriasis, or infections, leaves darker patches on the skin. Livedo reticularis appears as a net-like purplish discoloration from reduced blood flow, sometimes triggered by cold. Conditions like eczema and psoriasis can lead to red, brown, or purple patches that may linger after inflammation. Contact dermatitis, caused by allergic reactions, also leads to redness and discoloration.
Melanoma and other skin cancers may present as dark spots that change over time, requiring medical attention. Infections, like cellulitis or fungal issues, cause redness and dark patches. Vitiligo leads to white patches due to pigment loss, while acanthosis nigricans results in darkened, velvety skin, often linked to metabolic conditions like insulin resistance. These non-vascular causes of leg discoloration stem from trauma, inflammation, or pigment disorders, and persistent discoloration should be evaluated by a healthcare provider for an accurate diagnosis.
Radiofrequency ablation is a minimally invasive procedure. Your doctor will insert a catheter into an area of affected veins and use radiofrequency energy to heat the veins at a low temperature. This procedure reroutes blood to healthier vessels and rarely causes any postoperative pain.
Sclerotherapy is similar to radiofrequency ablation but uses a sclerosant chemical solution to reroute the blood flow instead of a catheter and radiofrequency.
Is Leg Discoloration Serious?
Yes, leg discoloration can indicate an underlying vascular issue that may need treatment. While it might start as a cosmetic issue, discoloration due to circulatory problems can worsen if left untreated.
Chronic venous insufficiency, one of the leading causes of leg discoloration, can result in serious complications, including venous ulcers, infections, and even deep vein thrombosis. These complications can significantly impact quality of life, causing pain, discomfort, and difficulty with mobility.
If your leg discoloration is accompanied by swelling, pain, or visible varicose veins, it's essential to seek medical attention. Early diagnosis and treatment can prevent the condition from progressing and help manage symptoms effectively.
While home remedies can help alleviate some of the discomfort associated with leg discoloration, they are not a substitute for professional medical treatment, primarily when the underlying cause is related to vascular issues.
If your leg discoloration is mild and you’re not experiencing significant pain or discomfort, there are several ways to manage the condition at home:
Compression Stockings
Wearing compression stockings can help improve blood flow in your legs by applying gentle pressure, reducing swelling, and preventing blood from pooling in your veins.
Elevating Your Legs
Elevating your legs above the level of your heart for short periods throughout the day can help reduce swelling and improve circulation.
Regular Exercise
Walking, swimming, and other low-impact exercises can improve leg circulation and help manage venous insufficiency symptoms.
Moisturizing
Keeping the skin on your legs moisturized can help prevent the dryness and itching often associated with venous stasis dermatitis.
While these methods can help manage symptoms, they do not treat the root cause of leg discoloration. It’s essential to consult a doctor for a thorough evaluation to ensure you receive the proper care.
Think you may have leg discoloration?
Managing Leg Discoloration After Treatment: Strategies for Home Care
Following your treatment, your healthcare provider may advise incorporating certain practices at home to complement the clinical interventions.
Making healthy lifestyle modifications can help manage leg discoloration. Staying at a healthy weight and focusing on consistent physical activity can significantly improve your recovery. It's essential to avoid tight-fitting garments that could impede circulation and opt for compression stockings if your healthcare professional suggests them.
What Are My Treatment Options for Leg Discoloration?
When treating leg discoloration caused by vascular issues, your doctor will evaluate the underlying cause and recommend treatment based on your specific condition. Common treatments include:
Radiofrequency Ablation
This minimally invasive procedure uses heat to close off the damaged veins, redirecting blood flow to healthier veins. Over time, the closed vein shrinks and the discoloration fades.
Sclerotherapy
Sclerotherapy involves injecting a solution into the affected vein, causing it to collapse and eventually disappear. This treatment is often used for smaller varicose veins and spider veins.
Compression Therapy
Compression stockings or wraps apply pressure to the legs, helping improve circulation and reduce swelling.
Medications
In cases of blood clots, anticoagulants (blood thinners) like warfarin or heparin may be prescribed to reduce the risk of further clotting and improve blood flow.
Topical Treatments
Steroid creams or antihistamines may reduce inflammation and itching associated with venous stasis dermatitis.
What Happens If You Don’t Treat Leg Discoloration?
If leg discoloration caused by venous insufficiency is left untreated, the condition can progress and lead to more severe complications. Over time, the skin may become harder, thicker, and more prone to ulcers, and open sores that can become infected. These ulcers can be difficult to treat and may take a long time to heal.
In some cases, untreated venous insufficiency can result in deep vein thrombosis (DVT), a life-threatening condition in which a blood clot forms in the deep veins of the leg. If the clot breaks free and travels to the lungs, DVT can lead to a pulmonary embolism.
Ignoring the signs of leg discoloration and its underlying causes can significantly affect your mobility, comfort, and overall health. Early intervention is crucial to preventing these complications.
After receiving treatment for leg discoloration, it’s essential to follow your doctor’s recommendations for home care to manage symptoms and prevent recurrence. Here are a few strategies:
- Maintain a Healthy Weight
- Stay Active
- Wear Compression Stockings
- Moisturize Regularly
By combining clinical treatments with healthy lifestyle habits, you can manage leg discoloration effectively and improve your overall vascular health.
Seeking Help for Leg Discoloration at the Center for Vascular Medicine
At Center for Vascular Medicine, we specialize in diagnosing and treating vascular conditions that cause leg discoloration. Our team of vascular specialists is dedicated to providing comprehensive care for patients with venous and arterial diseases affecting the lower extremities. We are here to help you manage your condition and improve your quality of life.
If you’ve noticed changes in the color of your legs or are experiencing symptoms like swelling, pain, or varicose veins, schedule a consultation with our experts to get the care you need. Schedule an appointment at a Center for Vascular Medicine near you.
Ready to speak with a vascular specialist?