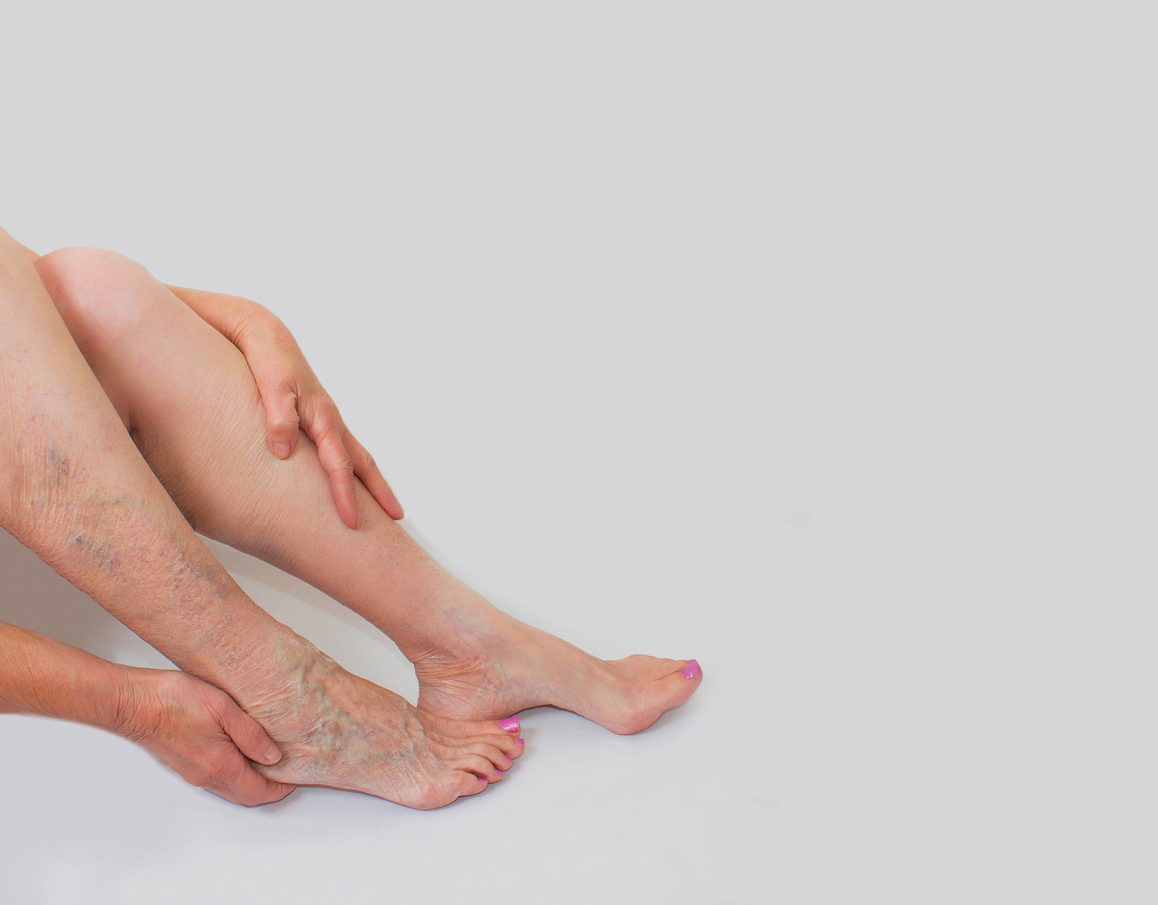
Types of Vascular Disease of the Legs
There are many types of vascular diseases that can occur in the legs – below are some of the common ones that can be treated at the Center for Vascular Medicine and the cause of the disease. You can generalize these diseases as failures to transport blood to or from key areas of the body. It is best to treat these diseases as early as possible to avoid future complications.
- Peripheral Artery Disease (PAD). PAD is caused by a chronic narrowing or blockage in the arteries and can lead to several problems, including cramps, pain, sores, skin-color changes and ulcers. In the most severe cases, called critical limb ischemia (CLI), amputation may be needed.
- Pelvic Congestion Syndrome (PCS). PCS is caused by the pooling of blood in your pelvis due to insufficient outflow. This typically leads to symptoms in the pelvis but can exacerbate symptoms in your lower extremities as well.
- May-Thurner Syndome (MTS). MTS is defined by compression of the left common iliac vein by the right common iliac artery. This compression narrows the left common iliac vein and reduces the amount of blood that can be circulated out of your legs.
- Chronic Venous Insufficiency. CVI is commonly caused by the failure or degradation of the valves in your veins. Some common symptoms of CVI include varicose veins and spider veins.
- Deep Vein Thrombosis (DVT). DVT occurs when a blood clot develops deep in a vein. This can be life-threatening if part of or the whole clot dislodges and travels to the lung. This is called a pulmonary embolism and you should seek urgent medical attention.
- Post-Thrombotic Syndrome (PTS). PTS typically occurs as a result of a DVT or other trauma that causes damage to the valves in your veins. When your valves are damaged, blood pools because it is less efficiently circulated out of your legs.
Arterial Versus Venous Vascular Diseases
Your vascular system is responsible for ensuring the proper transport of oxygen, and other nutrients to all parts of your body. This Lsystem is typically broken down into two main groups:
- Arteries carry oxygenated blood away from your heart.
- Veins carry this blood back to the heart so it can be recirculated.
There are many diseases that can affect this system and, while most are not immediately life-threatening, you should seek medical advice if you have any of the pertinent symptoms because these symptoms can quickly get worse. Particularly in the legs, some common symptoms include:
- Arterial symptoms - These are symptoms that show the patient may have an arterial issue. Coldness in legs, numbness of legs, tingling of legs, tingling when walking
- Venous symptoms - These are symptoms that show the patient may have a venous issue. Restless legs, restless legs at night, visible varicose veins, leg swelling, feet swelling, and leg pain during exertion.
Along with a comprehensive physical exam, the healthcare providers also look at risk factors as well including:
Arterial risk factors - smoking, diabetes, high blood pressure, high cholesterol. A patient smoking with diabetes is 8 times more likely to have arterial disease.
Venous risk factors - Obesity, genetics, multiple pregnancies.
Are you ready to speak with a vascular specialist?
Treatment options
Fortunately, the vascular problems that we have listed can be treated, but it is best to seek treatment early to avoid irreversible damage. Whether the damage is venous or arterial, many of the treatment options are similar.
Like with most other diseases, the first step is often to make lifestyle changes such as eating a healthy diet and exercising more often. Smoking cessation is also frequently recommended because it has been closely linked with the development of vascular diseases. Other lifestyle changes often include paying closer attention to blood sugar levels, blood pressure, and cholesterol.
There are some medications that can be prescribed to modulate factors that affect the vascular system. These include cholesterol medications, blood pressure medications, and blood thinners.
Invasive surgeries can be used to repair damaged veins and arteries. Vascular surgery involves grafting a blood vessel from elsewhere in the body to the area affected by the disease. Due to new innovations and developments of endovenous treatment modalities, vascular surgery is typically reserved for the most severe cases of vascular disease. Center for Vascular Medicine specializes in these newer endovenous modalities.
Newer treatment options
- Atherectomy procedure involves the mechanical removal of plaques or other blockages in your arteries. This is accomplished utilizing specialized medical devices.
- Angioplasty procedure and venoplasty procedure are similar in that a balloon is deployed and inflated in a diseased vessel to increase blood flow. When this occurs in an artery, the procedure is called an angioplasty and, when this occurs in a vein, the procedure is called a venoplasty. The balloon is deflated and removed after use.
- Many vessels, even after they have been opened up, no longer have the strength to remain open on their own so angioplasty and venoplasty are often done in conjunction with stenting. Stenting can occur in both veins and arteries and involves the permanent deployment of a metal scaffold to help keep the desired vessel open to blood flow.
Prognosis after Treatment
Vascular diseases progress and worsen over time so early diagnosis and treatment have been found to yield better long-term results. We typically see patient improvements about 1-4 weeks after initial treatment, but additional treatment is occasionally needed.
While complications are extremely rare, they can occur. The most common include minor bleeding from the sites used to access your vasculature. Lower back pain is expected and should not be of concern unless it persists for greater than 2 weeks.
What Happens When You Delay Treatment
Mild symptoms can worsen over time and become lifestyle limiting if left untreated some problems can include losing hair on the legs, wounds that will not heal, and persistent pain in the toes and feet. Some people experience thick, opaque toenails, restricted mobility, and impotence from slow circulation in their legs. Skin can become thin, shiny, and brittle. Pulses also weaken, and muscles become heavy, weak, and numb. The symptoms that develop and worse depending on the type of disease.
Some comorbidities increase the chances of vascular diseases in the legs. People who are overweight, diabetic, smokers, or physically inactive are also more likely to have blood circulation issues in their legs and feet.
What To Expect From CVM?
At the Center for Vascular Medicine, our mission is to help patients with their vascular diseases in a cost-effective and compassionate manner. We specialize in the diagnosis and treatment of venous and arterial diseases in the legs, feet, and pelvis. Our world-class providers are the most experienced in the specialty and work with patients to develop a treatment plan that is custom-tailored to their unique situation.
Typically, this process involves an initial consultation and ultrasound scan at one of our accredited facilities. After reviewing the results of your scan and obtaining a thorough medical history, our providers will discuss the results with you and help you decide on the next steps.
Our health care providers use several diagnostic tests to help determine what vascular diseases may be causing your symptoms. Our initial evaluations utilize ultrasound because this non-invasive imaging modality helps us verify our suspicions on whether your symptoms are caused by underlying vascular disease.
However, ultrasound alone cannot confirm a diagnosis. The gold standard of diagnosis in our field includes venogram procedure, angiogram, and intravascular ultrasound (IVUS). These imaging modalities are more invasive so we always opt to begin with ultrasound before recommending further evaluation. If you are recommended a procedure, our provider team will go through all of your options in detail and provide all the information you need to be prepared and to make an informed decision.
Are you ready to speak with a vascular specialist?