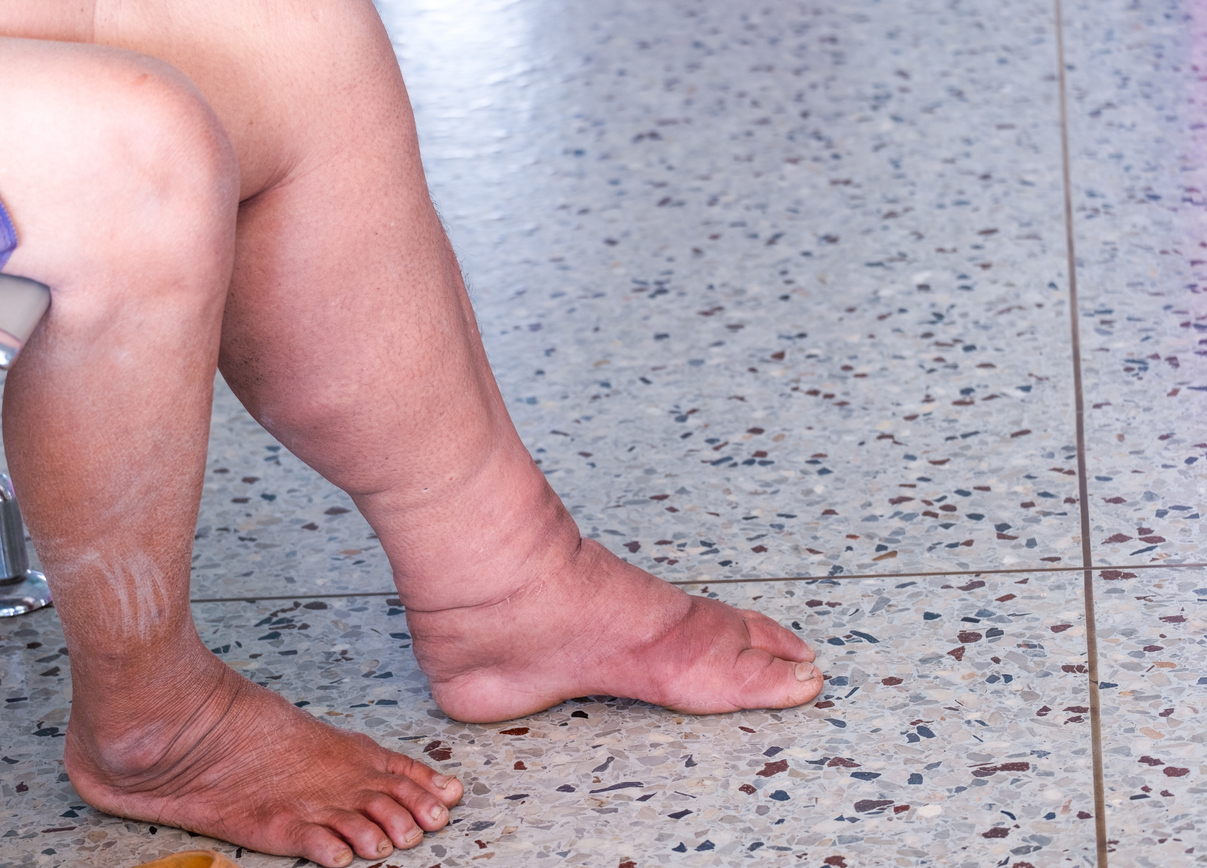
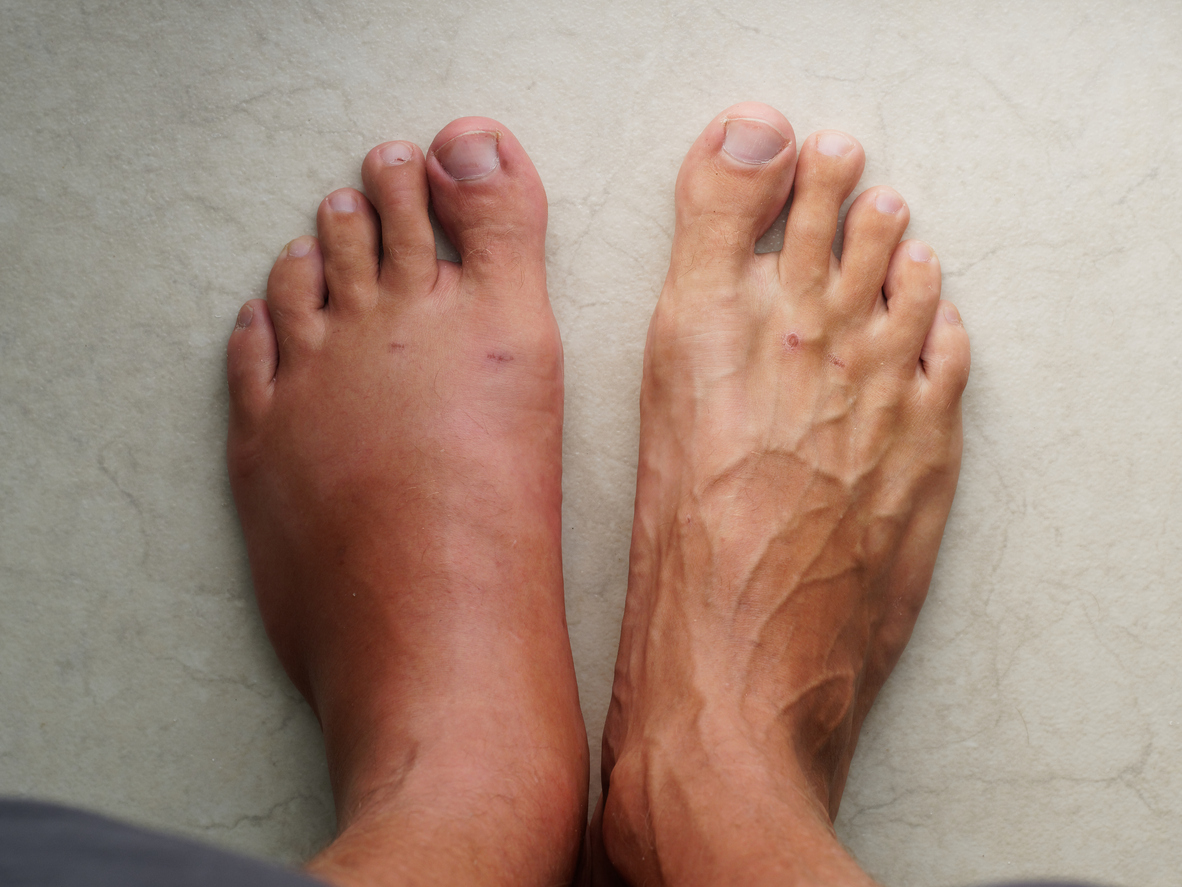
What Causes Leg Discoloration and Swelling?
Leg problems such as swelling and discoloration affect many people worldwide. One of the primary causes of these issues is peripheral vascular disease (PVD). To effectively treat these problems, it is essential to understand the intricate dynamics of leg discoloration and edema (swelling). These symptoms often indicate underlying vascular disease and require immediate attention and tailored interventions.
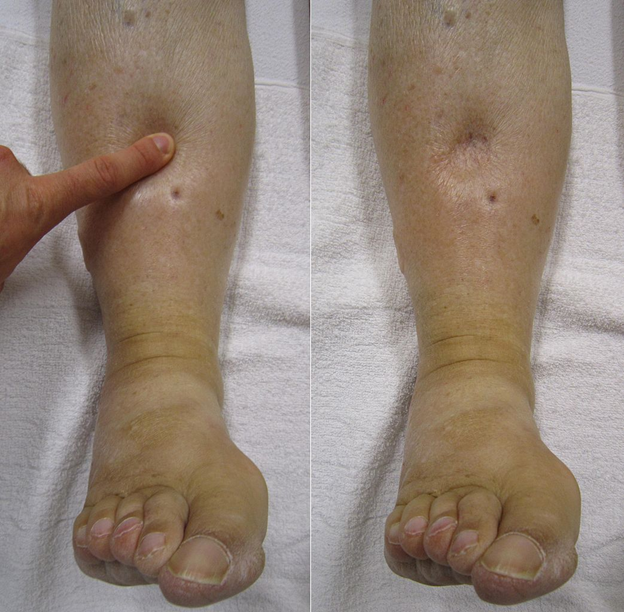
Licensed by CC 3.0 Image by James Heilman, MD via Wikimedia Commons
Leg discoloration and swelling in the legs can stem from various underlying causes, including vascular, lymphatic, inflammatory, and systemic conditions. Here are some common factors:
Deep Vein Thrombosis (DVT): DVT is a condition where a blood clot forms in a deep vein, typically in the legs. The clot can obstruct blood flow, causing swelling, pain, and potentially skin discoloration due to impaired circulation.
Peripheral Arterial Disease (PAD): A narrowing or blockage of the leg arteries, which reduces blood flow to the lower extremities. This can result in swelling and skin changes, such as pallor or bluish discoloration, particularly during physical activity.
Lymphedema: Lymphedema is a condition characterized by swelling caused by a buildup of lymphatic fluid in the tissues. It can be primary (congenital) or secondary (acquired), often resulting from lymph node removal, radiation therapy, infection, or trauma. Skin discoloration may occur due to chronic inflammation and tissue damage.
Chronic Venous Insufficiency (CVI): CVI refers to long-term venous insufficiency, leading to chronic swelling, skin changes, and potential ulcer formation in the lower legs. The increased pressure in the veins can cause fluid leakage and tissue damage, contributing to discoloration.
Infection or Inflammation: Infections or inflammatory conditions affecting the legs, such as cellulitis or vasculitis, can lead to localized swelling, redness, and skin discoloration due to inflammation and immune response.
Heart Failure: Chronic heart failure can result in fluid retention and swelling in the legs, known as peripheral edema. This swelling may be accompanied by skin discoloration due to poor circulation and impaired tissue perfusion.
Medications: Certain medications, such as calcium channel blockers, corticosteroids, or nonsteroidal anti-inflammatory drugs (NSAIDs), may cause fluid retention and swelling in the legs as a side effect.
Trauma or Injury: Trauma or injury to the legs, such as fractures, sprains, or contusions, can lead to localized swelling and bruising (discoloration) due to tissue damage and inflammation.
Pregnancy: Hormonal changes and increased pressure on the veins during pregnancy can cause fluid retention and swelling in the legs (edema), along with skin changes and discoloration.
If you have persistent or worrying symptoms, it's important to seek the advice of a healthcare professional for a proper assessment and diagnosis. Treatment will be based on the underlying cause and may involve lifestyle changes, medications, compression therapy, or other medicines.
Edema in the lower legs can manifest through various symptoms, indicating tissue buildup. Common symptoms include:
Swelling: Noticeable swelling, often beginning at the ankles and gradually extending upward, is a primary symptom of lower leg edema. The affected area may appear puffy or feel tight and stretched.
Skin Changes: The skin in the affected area may exhibit tightness, shininess, or increased warmth. It may also appear stretched or feel tender to the touch.
Discoloration: Edema can cause changes in skin color, ranging from pale or reddish to bluish or purplish hues. These discolorations may be localized or spread across the affected area.
Reduced Mobility: Severe edema can limit movement and flexibility in the lower legs, making it challenging to walk or stand for extended periods.
Pain or Discomfort: Edema-related swelling can lead to sensations of heaviness, achiness, or discomfort in the affected legs. This discomfort may worsen with prolonged standing or sitting.
Pitting Edema: Pressing a finger into the swollen area may leave a temporary indentation or "pit" that persists for a few seconds to minutes, indicating pitting edema.
Restricted Circulation: In advanced cases, edema can impair blood flow, leading to numbness, tingling, or a feeling of heaviness in the legs.
If you experience persistent or worsening symptoms of edema in your lower legs, consult a healthcare professional. These symptoms may indicate underlying health issues requiring evaluation and treatment.
What’s the Connection Between Edema and Leg Discoloration?
Compromised circulation disrupts the delicate balance within the skin. When blood flow is impaired, tissues may not receive enough oxygen, leading to a bluish discoloration (cyanosis).
For patients with chronic venous insufficiency, faulty valves allow blood to pool, increasing pressure and causing fluid leakage. This leakage can lead to swelling (edema) and a reddish or brownish discoloration from hemosiderin, a breakdown product of hemoglobin that accumulates in the tissues.
Reduced blood flow can also cause tissue hypoxia (oxygen deficiency) and ischemia (lack of blood supply), damaging tissues and contributing to skin discoloration, such as a mottled appearance or purplish color.
Compromised circulation can trigger inflammation, leading to redness (erythema) and discoloration. In deep vein thrombosis (DVT), blood clots can obstruct flow and cause stagnation, leading to localized swelling and discoloration.
Lymphatic dysfunction, as seen in lymphedema, can worsen circulation and contribute to discoloration by causing fluid buildup, inflammation, and skin texture and pigmentation changes.
Overall, compromised circulation disrupts the delivery of oxygen and nutrients to the skin, leading to a cascade of effects, including hypoxia, inflammation, fluid retention, and skin discoloration. Recognizing and treating the underlying vascular problems is crucial for managing these discolorations and preventing further complications.
When Should I Talk to My Vascular Specialist About Leg Swelling and Changes to My Skin?
It's essential to talk to your vascular specialist about leg swelling and changes to your skin if you notice any persistent or concerning symptoms. Here are some indicators that your symptoms warrant medical attention:
Persistent Swelling: If you experience persistent swelling in one or both legs that doesn't improve with elevation or rest, it's essential to consult your vascular specialist. This could be a sign of underlying vascular or lymphatic issues that require evaluation and treatment.
Skin Changes: Any changes in the color, texture, or appearance of your skin, especially in conjunction with swelling, should be evaluated by a healthcare professional. This includes redness, blueness, ulceration or purplish discoloration, as well as skin that feels tight, shiny, or unusually warm.
Pain or Discomfort: If you experience pain, discomfort, or aching sensations in your legs, particularly in combination with swelling or skin changes, it's essential to seek medical attention. These symptoms could indicate underlying vascular or inflammatory conditions that require assessment and management.
Difficulty Walking or Standing: Difficulty walking, standing, or performing daily activities due to leg swelling or discomfort may indicate significant underlying issues that warrant medical evaluation. This could include conditions such as chronic venous insufficiency, peripheral artery disease, or deep vein thrombosis.
History of Vascular or Heart Disease: If you have a history of vascular or heart disease, including conditions such as chronic venous insufficiency, peripheral artery disease, or heart failure, it's essential to monitor any changes in your legs closely and consult your vascular specialist if you notice new or worsening symptoms.
Recent Trauma or Surgery: If you have recently experienced trauma or undergone surgery involving your legs, any new swelling, skin changes, or pain should be promptly evaluated by a healthcare professional to rule out complications such as blood clots or infection.
If you have any concerns about leg swelling or changes to your skin, it's best to err on the side of caution and consult your vascular specialist for further evaluation and guidance.
Your Center for Vascular Medicine board-certified specialist can work with you to provide comprehensive care that targets the underlying vascular dysfunction, alleviates symptoms, and improves overall vascular health by addressing the root causes of edema and leg discoloration.
Think you may have vascular symptoms of leg or ankle swelling?
Diagnosis and Treatment
Accurate diagnosis entails comprehensive evaluations, encompassing detailed medical history, thorough physical examination, and diagnostic tests such as venous Doppler studies and venography. At Center for Vascular Medicine, treatment plans are meticulously tailored to our patient’s needs, considering factors such as age, overall health, and severity of symptoms.
Conservative management often entails lifestyle adjustments like leg elevation and compression stockings, complemented by medical interventions such as venous ablation or lymphedema therapy. Pregnant women grappling with leg swelling are advised specific measures like elevation and compression stockings.
Prognosis and Prevention for Leg Swelling
Timely diagnosis and adherence to treatment plans are pivotal for symptom management and reducing complications. Long-term management entails sustained lifestyle modifications, regular exercise, and vigilant monitoring of medical conditions.
Golden-Standard Care with Center for Vascular Medicine
Center for Vascular Medicine (CVM) specializes in diagnosing and treating venous and arterial diseases affecting the legs, feet, and pelvis. Our seasoned providers craft personalized treatment plans tailored to each patient's needs, harnessing advanced diagnostic techniques like ultrasound imaging.
Leg discoloration and edema can significantly impair quality of life, but we ensure our patients can effectively manage their symptoms with timely intervention and comprehensive care. Individuals can reclaim comfort and mobility by unraveling the underlying causes and seeking appropriate medical attention, enhancing their overall well-being. Book online at one of our Virginia, New Jersey, or Maryland offices!
Are You Ready to speak with a vascular specialist?