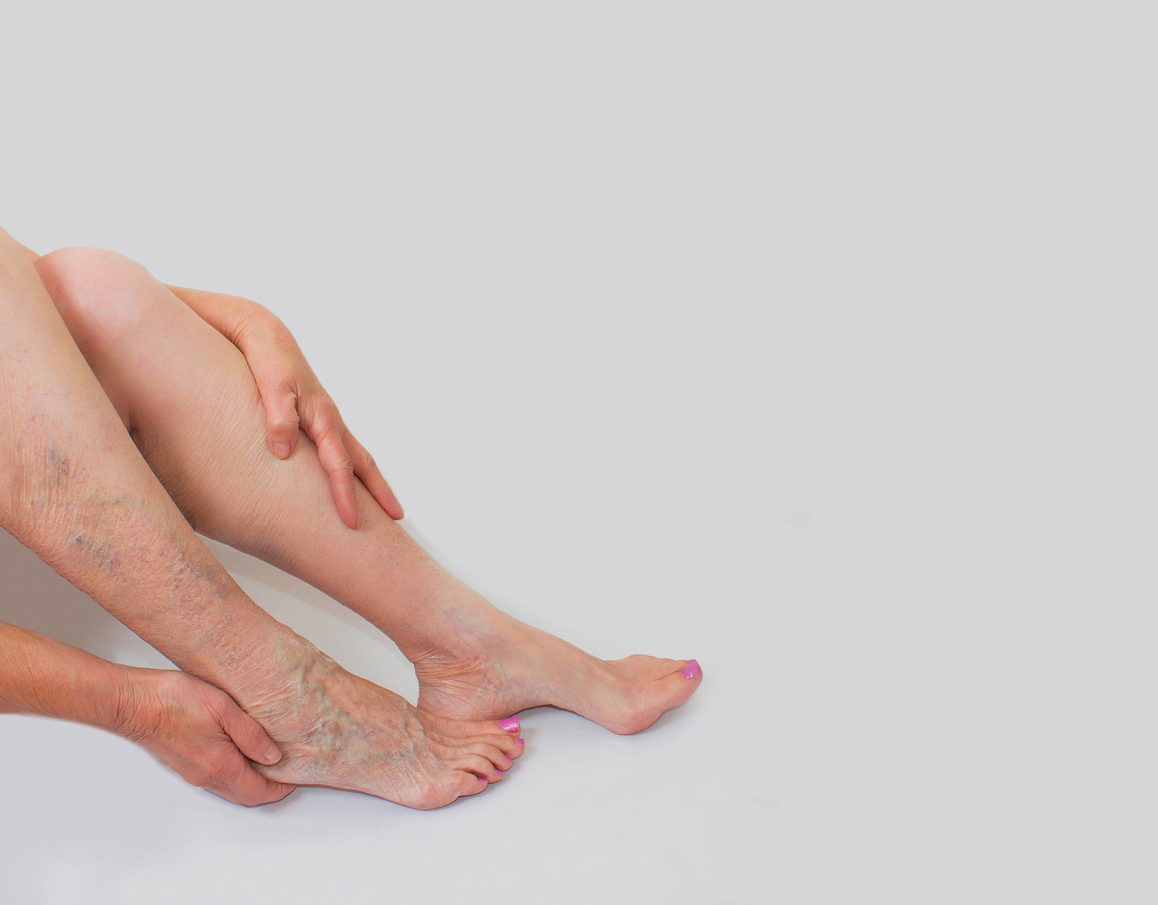
Types of Vascular Disease of the Feet
There are many types of vascular diseases that can occur in the legs – below are some of the common ones that can be treated at the Center for Vascular Medicine and the cause of the disease. You can generalize these diseases as failures to transport blood to or from key areas of the body. It is best to treat these diseases as early as possible to avoid future complications.
- Peripheral Artery Disease (PAD). PAD is caused by a chronic narrowing or blockage in the arteries and can lead to several problems, including cramps, pain, sores, skin-color changes and ulcers. In the most severe cases, called critical limb ischemia (CLI), amputation may be needed.
- Pelvic Congestion Syndrome (PCS). PCS is caused by the pooling of blood in your pelvis due to insufficient outflow. This typically leads to symptoms in the pelvis but can exacerbate symptoms in your lower extremities as well.
- May-Thurner Syndome (MTS). MTS is defined by compression of the left common iliac vein by the right common iliac artery. This compression narrows the left common iliac vein and reduces the amount of blood that can be circulated out of your legs.
- Chronic Venous Insufficiency (CVI). CVI is commonly caused by the failure or degradation of the valves in your veins. Some common symptoms of CVI include varicose veins and spider veins.
- Deep Vein Thrombosis (DVT). DVT occurs when a blood clot develops deep in a vein. This can be life threatening if part of or the whole clot dislodges and travels to the lung. This is called a pulmonary embolism and you should seek urgent medical attention.
- Post-Thrombotic Syndrome (PTS). PTS typically occurs as a result of a DVT or other trauma that causes damage to the valves in your veins. When your valves are damaged, blood pools because it is less efficiently circulated out of your legs.
Arterial Versus Venous Vascular Disease
Vascular diseases involve damage to the blood vessels in your feet. The damage reduces blood circulation, and this lowers healing capabilities and general foot health.
Your vascular system is responsible for ensuring the proper transport of oxygen, and other nutrients to all parts of your body. This system is typically broken down into two main groups:
- Arteries carry oxygenated blood away from your heart.
- Veins carry this blood back to the heart so it can be recirculated.
Along with a comprehensive physical exam the healthcare providers also look at risk factors as well including:
- Arterial risk factors - smoking, diabetes, high blood pressure, high cholesterol. A patient smoking with diabetes is 8 times more likely to have an arterial disease.
- Venous risk factors - Obesity, genetics, multiple pregnancies.
Signs & Symptoms of Vascular Disease
There are many diseases that can affect this system and, while most are not immediately life-threatening, you should seek medical advice if you have any of the pertinent symptoms because these symptoms can quickly get worse. Particularly in the legs, some common symptoms include:
- Arterial symptoms - These are symptoms that show the patient may have an arterial issue. Coldness in feet, numbness in legs and feel, tingling of legs and feet, tingling when walking.
- Venous symptoms - These are symptoms that show the patient may have a venous issue. Restless feet, restless legs and feet at night, visible varicose veins, leg swelling, feet swelling, and leg pain during exertion.
Symptoms of potential vascular disease in the feet include:
- Pain when walking or exercising.
- Pain when resting across the top of the foot and toes. If you elevate your feet, the problem gets worse.
- Ulcers and possibly gangrene.
- Pale feet when elevated.
- Discolored feet.
- Feet swelling
- Difficulty in moving toes and flexing feet.
- Low or no pulse in the foot.
- Sensations of numbness or tingling.
Peripheral vascular disease or peripheral artery disease develops slowly, but if left untreated, increases in severity, and diminishes your quality of life.
Risk Factors
Your lifestyle choices impact the health of your vascular system. The significant risk factors are:
- Smoking
- Diabetes
- High blood pressure.
- High cholesterol
- Age
The first approach to preventing or reducing the impact of vascular disease in your feet is to minimize your risk factors by:
- Quitting smoking
- Manage your diabetes and look after your feet.
- Medication to reduce your high blood pressure.
- Medication and change in diet to reduce cholesterol.
- Losing weight, reducing alcohol consumption, and exercising to counter the effects of aging.
Complications of Vascular Disease in Feet
It's not just your feet that suffer from the process that causes peripheral vascular disease - the feet are indicators of what is going on in the rest of your body. The consequences of clogged and blocked arteries and veins are life threatening.
Vascular disease of the foot means you are more likely to develop or have:
- Cardiovascular disease
- Critical limb ischemia.
Are you ready to speak with a vascular specialist?
Treatment Options
There is no cure for vascular disease in the feet, and all treatment options aim to reduce the impact of your symptoms to try to avoid developing complications resulting in a heart attack, stroke, or potential limb amputation.
The treatment options include one or more of the following:
- Lifestyle changes
- Medication
- Surgery
The newer treatment options include atherectomy, stenting, angioplasty and venoplasty.
- Atherectomy Procedure involves the mechanical removal of plaques or other blockages in your arteries. This is accomplished utilizing specialized medical devices.
- Angioplasty Procedure and venoplasty procedure are similar in that a balloon is deployed and inflated in a diseased vessel to increase blood flow. When this occurs in an artery, the procedure is called an angioplasty and, when this occurs in a vein, the procedure is called a venoplasty. The balloon is deflated and removed after use.
- Many vessels, even after they have been opened up, no longer have the strength to remain open on their own so angioplasty and venoplasty are often done in conjunction with stenting. Venous Stenting can occur in both veins and arteries and involves permanent deployment of a metal scaffold to help keep the desired vessel open to blood flow.
Lifestyle Changes
Smoking causes lung cancer and increases your risk of heart disease and strokes. It also contributes to vascular disease and the risk of amputation. The nicotine in tobacco causes the blood vessels to constrict. Narrow blood vessels attract deposits of plaque, and this further restricts blood flow. Vascular disease is the impact of restricted blood flow with pain, swelling, and soft tissue death. However old you are, stopping smoking is the most significant way to improve your health and live longer.
The second lifestyle change is increasing your exercise. You may think that if your feet hurt that walking is the worse thing you can do. The modern approach to exercising with Peripheral Arterial Disease (PAD) aims for you to walk as far as you can every day using a stop and start process. Your physician may prescribe supervised exercise to get you started.
Finally, there is the standard lifestyle hangs that everyone knows will improve your health:
- Eat well.
- Reduce alcohol.
- Get enough sleep.
- Lose weight.
Medication
You don't need all the medicines available but a combination of one or two to treat your symptoms and help improve your blood flow. The medication you need depend on your:
- Blood pressure.
- Cholesterol levels.
- Risk of blood clots.
- Pain levels.
If you have an infection because of a foot ulcer, for example, then you may need antibiotics.
Surgery
Surgery to improve the condition of your blood vessels can be minimally invasive with the use of a catheter or may require more invasive procedures if performing a bypass operation.
The goal of surgery is to improve blood flow in your feet to keep your tissues healthy. The surgery will perform one or more of the following processes.
- Removing blockages.
- Increasing the diameter of the blood vessel.
- Reinforcing blood vessel walls.
- Providing an alternative route for blood flow.
There are always risks with any surgery, however minor, and your medical team will discuss these and the expected benefits.
Prognosis After Treatment
There is no cure for vascular disease, so you are committed to maintaining your foot health and managing your symptoms. Surgery gives immediate benefits in improving blood circulation, but these benefits are lost if you don't make the lifestyle changes necessary to promote better health.
Vascular Disease and Diabetes
Diabetes increases your risk of vascular disease. The high blood glucose level in your blood encourages plaque deposits. People with diabetes need to pay close attention to maintaining their foot health because they are more at risk of developing a problem.
Careful blood sugar management helps reduce the impact of diabetes on your vascular system.
Foot Disease Resulting from Vascular Disease
Although the vascular disease is the underlying cause of your foot problems, you may see the symptoms as separate medical issues.
Cellulitis is a bacterial infection of the skin. Bacteria can enter through a cut, swollen skin, or an open sore like an ulcer. Although cellulitis is not a direct vascular disease, the impact of poor blood circulation makes wounds on your foot slow to heal. The longer you have an injury on your foot, the greater the chance of a bacterial infection. Plus, you may experience swelling in your foot as a direct result of vascular disease.
Bacterial infections, like cellulitis, usually respond well to antibiotics.
Swollen, puffy feet make it difficult to walk and make footwear uncomfortable. Tight shoes and socks can rub and cause damaged spots on your feet that may lead to an ulcer or chronic wound. Living with swollen feet is painful and can lead to a decrease in your quality of life and a loss of mobility.
Vascular disease means foot ulcers are slow to heal, may not heal, and may return frequently. Ulcers can result in deep sores and infections. Ulcers can take between six and twelve weeks to treat. Painful weeping sores on your feet are challenging to live with and make it difficult for you to take regular exercise.
Your blood nourishes your cells and takes away waste products; without blood, your cells can die and rot - gangrene. Ultimately gangrene leads to removal of the dead tissue and possible amputation of your foot
Poor circulation can result in frostbite in your toes in freezing weather. Severe frostbite means loss of toes.
Although discolored feet look like a disease, they are often an indication of peripheral artery disease (PAD) and the potential complications of vascular disease in the foot.
Are you ready to speak with a vascular specialist?