Post-Thrombotic Syndrome Patient Guide
Post-thrombotic syndrome (PTS) is a severe and painful condition that develops as a long-term complication following deep vein thrombosis (DVT). The veins in your legs and arms contain small valves that ensure blood flows appropriately back to the heart. When DVT occurs, a clot forms that blocks these valves, disrupting blood flow and causing significant valve damage.
Symptoms of post-thrombotic syndrome can include chronic pain, swelling, and other symptoms in the affected limb, most commonly the legs. Due to ongoing discomfort and functional limitations, this condition can significantly impact the quality of life, making early detection and management crucial to reducing the risk of PTS.
Over a third of individuals with DVT will develop PTS, experiencing symptoms such as ulcers, chronic leg pain, swelling, and redness. If you’ve experienced a DVT or similar vascular event, it’s essential to follow up with your vascular specialist, keep all appointments, and follow your treatment plans.
Am I at Risk for Post-Thrombotic Syndrome?
It is essential for patients who have had deep vein thrombosis (DVT) to understand their risk factors for developing post-thrombotic syndrome (PTS). Post-thrombotic syndrome affects about 50% of individuals who have had DVT in the legs. Potential factors for post-thrombotic syndrome include but aren’t limited to:
- Obesity or a BMI greater than 35
- History of DVT occurring above the knee (in the thigh or groin)
- No treatment, delayed treatment, or incomplete treatment of DVT
- A history of multiple DVTs
- Old age
- Pre-existing vein diseases, such as chronic venous insufficiency and varicose veins
Discuss your risks of developing post-thrombotic syndrome with your vascular specialist to stay proactive about your vascular health.
Long-term Effects of Post Thrombotic Syndrome
Over time, continuous pressure and improper blood flow can severely damage the skin on your legs. The skin may become dry, itchy, and discolored, particularly around the ankles. Without treatment, the skin can become stiff, leathery, and brown. Even minor cuts or abrasions in this area can develop into sores that do not heal, known as venous ulcers.
In severe cases, the vein may be so damaged that it becomes completely blocked, stopping blood flow.
Prevention and Management
Preventing PTS involves timely and effective treatment of DVT. This includes anticoagulant therapy and, in some cases, catheter-directed thrombolysis (CDT), which helps dissolve the clot and restore blood flow. Compression stockings can help manage symptoms but are not routinely recommended to prevent PTS. Regular follow-up and monitoring are essential to manage and mitigate the symptoms of PTS effectively.
By understanding these aspects and working closely with your healthcare provider, you can take steps to manage PTS and maintain a better quality of life.
What are the Symptoms of Post-Thrombotic Syndrome?
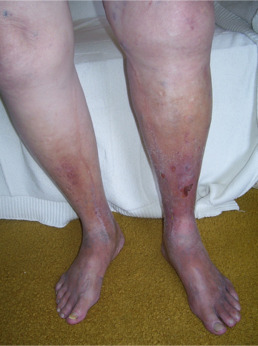
Post-thrombotic syndrome (PTS) can vary significantly in its impact, presenting minor symptoms in some cases and severe ones in others. Typically, the symptoms manifest in the same leg previously affected by deep vein thrombosis (DVT). Common symptoms include:
- Redness or darkening of the affected skin on the leg
- A feeling of heaviness in the leg
- Leg swelling
- Cramping, tingling, or itching in the leg
- Widening of the veins in the leg
- Leg pain that worsens when standing and improves when raising or resting the leg
- Sores or leg ulcers
If you notice these symptoms, especially following a recent DVT, it is essential to schedule an appointment with your vascular specialist.
How is Post-Thrombotic Syndrome Diagnosed?
You can often diagnose post-thrombotic syndrome (PTS) based on signs, symptoms, and medical history. If these align with PTS, additional testing may not be necessary. However, your vascular specialist might recommend blood work or an ultrasound of your legs to be thorough.
During the diagnostic process, your vascular specialist will discuss your medical history, especially if you’ve had a deep vein thrombosis (DVT). They will also inquire about your current symptoms and conduct a physical exam, focusing closely on your legs.
In some cases, further tests may be necessary to confirm the diagnosis. The most commonly used tests include blood tests to check for clotting issues or ultrasound imaging for visual detection of problems in the leg veins.
Your vascular specialist might use a Villalta score to assess the severity of your PTS. This scale rates the severity of your symptoms. A score of 15 or higher indicates a severe case of PTS.
Your Center for Vascular Medicine healthcare team is here to ensure you receive the most accurate diagnosis and effective care. Talk to your vascular specialist if you have any concerning symptoms after a vascular event like a DVT.
What are My Treatment Options for Post-Thrombotic Syndrome?
The treatment of post-thrombotic syndrome (PTS) depends on the severity of your condition. Generally, it includes a combination of leg elevation, compression therapy, exercise, and possibly medications to manage symptoms and prevent further complications.
Elevation
Elevating the affected leg above the heart can help alleviate symptoms of post-thrombotic syndrome. Special leg elevation pillows can make this more comfortable than struggling with cushions or pillows. Although you don’t need to sleep with your legs elevated, it’s beneficial to elevate them when relaxing at home until swelling decreases.
Elevating your leg while resting helps blood return to the heart, using gravity to reduce swelling. Simple exercises, such as flexing the ankle joint and engaging in activities that strengthen the calves, can help alleviate the symptoms of post-thrombotic syndrome.
Compression Stockings
Graduated compression stockings are a crucial part of PTS treatment. These specially designed garments improve blood flow, reduce swelling, and alleviate pain. Talk to your vascular specialist about what type and fit of compression stocking is right for you. Properly fitting compression stockings should be comfortable and practical to put on and take off, with assistive devices available if needed.
Medications
Your vascular specialist may provide blood thinners to prevent recurrent blood clots in the legs. Talk to your vascular specialist and primary care provider before taking any over-the-counter medications or supplements as remedies or preventatives for post-thrombotic syndrome, as certain supplements may interfere with existing medications.
Minimally Invasive Procedures
Your vascular specialist will take your medical history, risk factors, and history of DVT into consideration before recommending surgical intervention for post-thrombotic syndrome symptoms. For more severe cases of PTS, specific procedures may help alleviate symptoms:
Thrombectomy or Thrombolysis: These procedures dissolve or remove clots from the vein. They are especially effective when the clot is in its early stages and are commonly recommended for larger clots.
Venous Ablations or Sclerotherapy: These techniques close malfunctioning or damaged veins, redirecting blood flow through healthier veins.
Venoplasty and Venous Stenting: These procedures widen narrowed veins caused by scarring from a clot or external compression.
Your healthcare team is dedicated to providing the best care and support. If you have any questions or need further assistance, please don’t hesitate to contact your vascular specialist.
How Can I Prevent Post-Thrombotic Syndrome?
Post-thrombotic syndrome (PTS) can have a range of symptoms that may last for months or even years. For some people, these symptoms remain mild and stable, but for others, the condition can progress to the point where it becomes disabling. Fortunately, most patients can manage their symptoms appropriately and maintain healthy, active lives. Early treatment and following medical advice are crucial for success.
Patients can help reduce the risk of post-thrombotic syndrome (PTS) by avoiding prolonged periods of immobility, such as after surgery or due to a medical condition. If you are unable to move for long periods, your doctor can provide strategies to help prevent DVT. These strategies include:
- Walking and moving as soon as you’re cleared to
- Using compression devices
- Wearing prescription-grade compression stockings
- Taking blood-thinning medications as prescribed
Treating DVT promptly is the best way to prevent PTS. If prescribed, take your blood thinner medication and never miss a follow-up test to check your blood levels. Additionally, using compression stockings or other devices as your doctor recommends is essential.
Early symptoms of PTS include slight discomfort, redness, and itchiness in the legs. Over time, these symptoms can worsen, leading to increased pain, itchiness, and discoloration in the lower legs. The veins' walls and valves can suffer severe damage, resulting in irreparable scarring.
What Happens if Post-Thrombotic Syndrome Goes Untreated?
Without treatment, PTS can lead to immobility and other serious consequences. Therefore, seeking medical advice and adhering to treatment plans is essential to manage this condition effectively.
Chronic Pain and Discomfort
Persistent pain and swelling can severely impact daily life, making it difficult to perform everyday activities. This discomfort can also affect mobility, leading to complications such as muscle atrophy and decreased physical fitness.
Increased Risk of Recurrent DVT
Without proper management, PTS can lead to additional deep vein thrombosis, which complicates the venous system and increases the risk of pulmonary embolism—a potentially life-threatening condition. If you experience unexplained sudden pain in the leg or calf accompanied by warmth, redness, chest pain, dizziness, or confusion, this could indicate a deep vein thrombosis a medical emergency. Please seek immediate medical treatment.
Skin Changes and Ulcers
PTS can cause significant skin changes and ulcers. Chronic venous insufficiency can lead to skin discoloration, eczema, and the development of ulcers that are often difficult to heal. These ulcers can become infected, leading to more severe health issues.
Reduced Mobility and Function
Chronic or ongoing symptoms of PTS can also reduce mobility and function. Difficulty walking or standing for prolonged periods can lead to a more sedentary lifestyle, affecting overall physical fitness. Mobility limitations and chronic pain or discomfort can also affect one’s ability to engage in social activities, further impacting mental health.
Seeking timely medical advice and following a treatment plan can help manage symptoms, prevent complications, and improve overall health. If you suspect you have PTS, it is essential to consult with a healthcare provider for proper evaluation and treatment.
Expert Vascular Care at Center for Vascular Medicine
If you are struggling with vascular discomfort, have a history of DVT, or are experiencing symptoms of post-thrombotic syndrome, don't wait to seek help. Center for Vascular Medicine is here to provide expert care and support. Our specialized team is dedicated to diagnosing and treating vascular conditions to help you lead a healthier, more comfortable life. Schedule a consultation for more information, or find a location near you.
This article is a comprehensive overview of Post Thrombotic Syndrome. However, it should not take the place of speaking with a physician. If you are experiencing any of the symptoms listed above, or know someone who is, contact us today to schedule a consultation.
You can also view other vascular diseases below:
Peripheral Arterial Disease (PAD)
FAQs
Patients with PTS may see their condition improve with proper treatment; however, the symptoms may never go away completely. Most doctors will recommend being active daily and engaging in flexing movements to strengthen the calf muscles.
PTS may cause leg sores or ulcers. If this happens, professional wound care is necessary. Pentoxifylline and aspirin may help with the healing of ulcers. If the ulcer is infected, antibiotics may be required. More severe ulcers that do not improve with wound care therapy and medicines may require surgery to remove the tissue that is damaged.
There are several situations where you need to contact your doctor right away. These include:
- A warm, painful area or ulcer on the leg
- Signs of an infected ulcer on your leg
- DVT symptoms like warmth, pain, or swelling, and heavy legs.

