What is May-Thurner Syndrome?
May-Thurner Syndrome (MTS), also known as Iliac Vein Compression Syndrome, is a medical condition that predominantly affects women, particularly those between the ages of 20 and 45. This condition arises when the left iliac vein is compressed, significantly decreasing blood drainage from the left leg causing swelling and discoloration. This compression can result in the formation of a deep vein thrombosis (DVT), which is essentially a blood clot. If not addressed promptly, DVT can lead to severe complications, including restricted blood flow, pain, swelling, and even varicose veins in the affected leg.
MTS is typically observed on the left side of the body, though there have been reported cases where symptoms manifest on the right side. The compression of the iliac vein by the right common iliac artery is the primary cause of this condition. This compression restricts the drainage of blood from the lower extremities, making it more prevalent among women who have experienced pregnancy. It is rare among women who have not had children, though men can also develop MTS, albeit less frequently.
What Are the Symptoms of May-Thurner Syndrome?
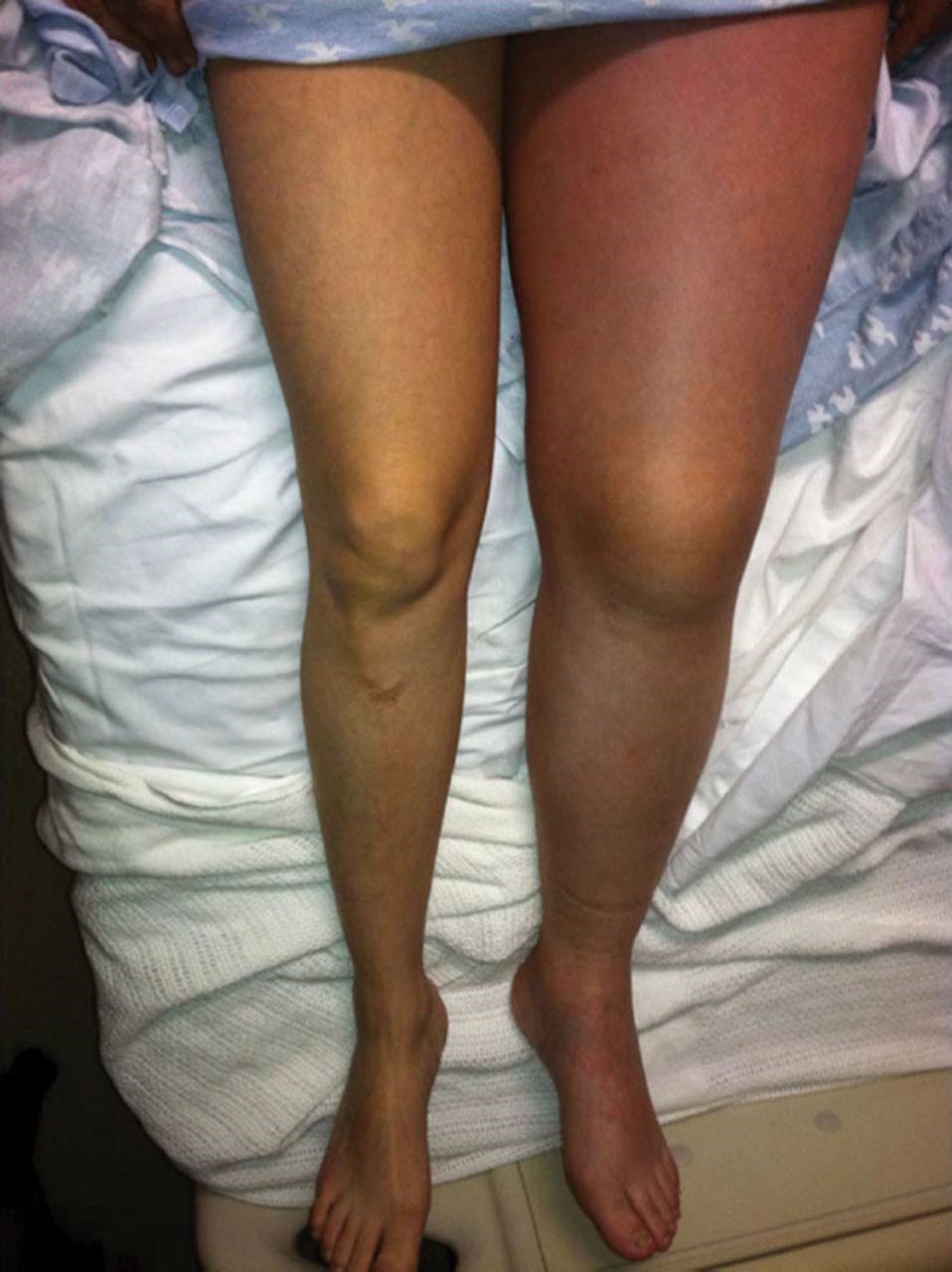
The symptoms of May-Thurner Syndrome can be varied and often develop gradually. Common signs and symptoms include generalized pelvic pain, painful swelling of the left leg, and the development of varicose veins, primarily affecting the left leg. The disorder is often triggered by prolonged periods of immobilization or after pregnancy. In some cases, patients may present with signs associated with post-thrombotic syndrome, such as pigmentation changes, chronic leg pain, phlebitis (inflammation of the veins), and recurrent skin ulcers.
Stage 1
Symptoms may be mild or absent in the early stages of May-Thurner Syndrome. As the condition progresses, patients may experience more pronounced symptoms. These can include generalized pain in the lower abdomen and pelvis, noticeable varicose veins in the upper leg (usually the left leg), swelling in the left leg, chronic leg pain that worsens throughout the day, and chronic hemorrhoids.
Stage 2
In Stage 2 of May-Thurner Syndrome (MTS), known as venous spur formation, the condition progresses to a more severe state from the initial vein compression (Stage 1). This results in the development of fibrous spurs or shelves within the iliac vein, further restricting blood flow and increasing the likelihood of deep vein thrombosis (DVT).
Patients with mild vein narrowing may not experience any symptoms. As the condition progresses, symptoms become more apparent and can significantly impact the quality of life. Pain and swelling associated with DVT can be severe, and the development of varicose veins can lead to additional complications such as leg ulcers and skin changes.
Stage 3
Stage 3 of May-Thurner Syndrome (MTS) is characterized by the development of deep vein thrombosis (DVT). This stage represents the most severe progression of the condition, where the compression of the iliac vein and the formation of fibrous spurs (Stage 2) has led to the formation of a blood clot within the vein. Stage 3 symptoms include but aren’t limited to:
Deep Vein Thrombosis (DVT): A blood clot forms in the iliac vein at this stage, severely restricting or completely obstructing blood flow from the leg. This clot formation directly results from the prolonged compression and narrowed blood flow caused by the fibrous spurs developed in Stage 2.
Severe Symptoms: The presence of a DVT can lead to significant and painful symptoms. Patients may experience intense pain and swelling in the affected leg, usually the left. The leg may feel heavy and warm, with noticeable redness or discoloration. Varicose veins can become more pronounced, and the pain often worsens with prolonged standing or walking.
Complications: One of the most dangerous complications of DVT is the risk of a pulmonary embolism (PE). If the blood clot breaks free from the vein, it can travel through the bloodstream and lodge in the lungs, blocking blood flow. This can cause severe chest pain, shortness of breath, rapid heartbeat, and even sudden death if not treated immediately.
How is May-Thurner Syndrome Diagnosed?
Diagnosing May-Thurner Syndrome involves a combination of non-invasive and minimally invasive tests. Patients often seek diagnosis after experiencing symptoms for several months or even years. Many patients are referred to vascular specialists by their primary care physicians or OB/GYNs after other conditions have been ruled out. Diagnosis usually includes a pelvic ultrasound, a CT venogram, and an intravascular ultrasound (IVUS) with venography.
A pelvic ultrasound is often the first step in diagnosing MTS. This non-invasive test uses sound waves to create images of the pelvic area, allowing doctors to see if there is any iliac vein compression. A CT venogram provides a more detailed look at the blood vessels in the pelvic region, using contrast dye to highlight any areas of compression or blockage. Intravascular ultrasound (IVUS) with venography is a more advanced diagnostic tool that combines ultrasound and X-ray imaging to provide a detailed view of the inside of the blood vessels.
Can May-Thurner Syndrome Be Treated?
Treatment for May-Thurner Syndrome varies based on the severity of the condition and the patient's specific needs. At the Center for Vascular Medicine, our approach is to provide the most conservative treatments that will deliver long-lasting relief. Most treatments for MTS are minimally invasive and are performed in an outpatient setting.
The standard treatments for May-Thurner Syndrome (MTS) include venoplasty, which uses a balloon catheter to open blocked veins, and iliac vein stenting, where a stent is inserted to keep the blood flow channel open. In more severe cases, bypass surgery, angioplasty, or repositioning of the right iliac artery may be necessary.
Can I Prevent or Decrease My Risk of May-Thurner Syndrome?
While it may not be possible to completely prevent May-Thurner Syndrome (MTS), several strategies and lifestyle changes can significantly reduce your risk and help manage the condition if you are already predisposed to it. Here’s an in-depth look at how you can prevent or decrease your risk of developing May-Thurner Syndrome:
Maintain a Healthy Weight
Maintaining a healthy body mass index (BMI) is crucial for reducing the risk of MTS. Excess weight can increase the pressure on your pelvic veins, potentially leading to compression. Keeping your weight within a healthy range can minimize this pressure and promote better venous health. A balanced diet rich in fruits, vegetables, lean proteins, and whole grains, combined with regular physical activity, can help you achieve and maintain a healthy weight.
Stay Active and Exercise Regularly
Regular exercise is vital for promoting good blood circulation and preventing blood clots. Activities that engage the calf muscles, such as walking, jogging, cycling, and swimming, are particularly beneficial. These exercises help pump blood from the legs to the heart, reducing the risk of venous stasis and clot formation. Aim for at least 30 minutes of moderate exercise most days of the week.
Avoid Prolonged Sitting or Standing
Prolonged sitting or standing can increase the risk of blood pooling in the legs, contributing to vein compression and clot formation. If your job requires long periods of sitting or standing, take regular breaks to move around and stretch. Flex your ankles, rotate your feet, and walk around whenever possible to promote blood flow. When traveling long distances by car or plane, stand up and move around every hour or so.
Wear Compression Stockings
Compression stockings or socks can help improve leg blood flow by applying gentle pressure. This pressure helps prevent blood from pooling and reduces the risk of clot formation. Compression stockings are beneficial during pregnancy, prolonged periods of standing or sitting, and long-distance travel. Talk to your vascular specialist to see if compression stockings suit you.
Manage Pregnancy-Related Risks
Pregnancy can increase the risk of MTS due to the added pressure on the pelvic veins. If you are pregnant, discuss with your healthcare provider the best ways to minimize this risk. Wearing compression stockings, staying active, and avoiding excessive weight gain during pregnancy can all help. Elevating your legs when sitting and sleeping on your left side can improve venous return and reduce pressure on the iliac veins.
Stay Hydrated
Proper hydration is essential for maintaining healthy blood viscosity and preventing blood clots. Dehydration can cause blood to thicken, increasing the risk of clot formation. Make sure to drink plenty of water throughout the day, especially during hot weather or when engaging in physical activity.
Wear Comfortable, Supportive Clothing and Footwear
High heels and tight clothing can impede blood flow from the legs to the heart, increasing the risk of vein compression and clot formation. Opt for comfortable, well-fitting shoes and clothing that allow proper circulation, especially in the summer heat.
Watch Your Posture
Specific postures, such as crossing your legs for long periods, can restrict blood flow and increase the risk of vein compression. Be mindful of your sitting and standing postures to ensure proper circulation. Elevating your legs above the level of your heart when resting can help reduce swelling and promote venous return. This is especially helpful if you experience leg discomfort or swelling after prolonged periods of standing or sitting.
Quit Smoking
Smoking is a significant risk factor for vascular diseases, including MTS. Quitting smoking can improve overall vascular health and reduce the risk of blood clots. If you need help quitting, consult your healthcare provider for resources and support.
Follow Through With All Treatment Plans and Medical Advice
If you undergo any surgical procedures, follow your doctor's advice for post-operative care to prevent complications related to blood clots. This may include wearing compression stockings, taking prescribed medications, and staying mobile as soon as it is safe.
Although May-Thurner Syndrome may not be entirely preventable, adopting these measures can significantly reduce your risk and help manage the condition if you are predisposed to it. Maintaining a healthy lifestyle, staying active, controlling weight, and using compression devices as recommended are all effective strategies.
Treat May-Thurner Syndrome At Center for Vascular Medicine
May-Thurner Syndrome is a progressive disease that can significantly impact a patient's quality of life if not diagnosed and treated early. However, with appropriate medical care, MTS can be managed effectively. While there is no cure for May-Thurner Syndrome, treatments can relieve symptoms and prevent complications. Most procedures are minimally invasive, allowing patients to return to normal daily activities with minimal downtime. Regular follow-ups with a healthcare provider are essential for monitoring the condition and ensuring that any additional areas of compression are treated promptly.
If you suspect that you have May-Thurner Syndrome or are experiencing symptoms such as leg pain, swelling, varicose veins, or chronic pelvic pain, it is essential to consult a healthcare provider. Early diagnosis and treatment can help prevent the disease's progression and improve overall quality of life. Contact our vascular specialists at the Center for Vascular Medicine to schedule a consultation or find a CVM location near you. You can manage the symptoms of May-Thurner Syndrome with appropriate treatment and maintain a healthy, active lifestyle.
FAQ
While there is no “cure” for May-Thurner Syndrome, it can be treated successfully to relieve symptoms. Most procedures are minimally invasive. With treatment, the patient can soon engage in their normal daily activities. However, regular follow-ups with a physician will be necessary. Although it is in a small percentage of patients, additional procedures may need to be done to treat additional areas of compression.
Some patients have reported fatigue, along with other symptoms, such as varicose veins and leg ulcers. If you feel exhaustion, accompanied by heaviness and swelling in your leg, it is vital to seek medical treatment immediately.
Patients with May-Thurner Syndrome may have persistent low back pain. The iliac vein’s narrowing will cause some patients to experience pain in their lower back, along with pelvic pain, bladder and bowel problems, bloating, and hemorrhoids. It is difficult to determine how much back pain is due to the iliac vein compression or other possible chronic back problems.

