Introduction
Many people ignore leg pain and assume they pulled a muscle, sprained something, or are experiencing arthritis symptoms. Many people feel that increased pain which may limit their activity is part of the natural aging process.
Peripheral arterial disease is when arteries or vessels are clogged and blood flow is restricted in your legs. While this might not seem like a big issue, it can result in heart attack, stroke, amputation, gangrene, and death. Leg pain when walking or climbing stairs may be a sign of peripheral arterial disease (PAD).
Let’s cover the importance of paying attention to leg pain, and we’ll go over some of the popular leg pain treatments.
Leg pain is often ignored or attributed to other causes, but it can be a sign of peripheral arterial disease (PAD) and should not be overlooked. This article will explore the importance of paying attention to leg pain and discuss popular treatment options for leg pain related to vascular disease.

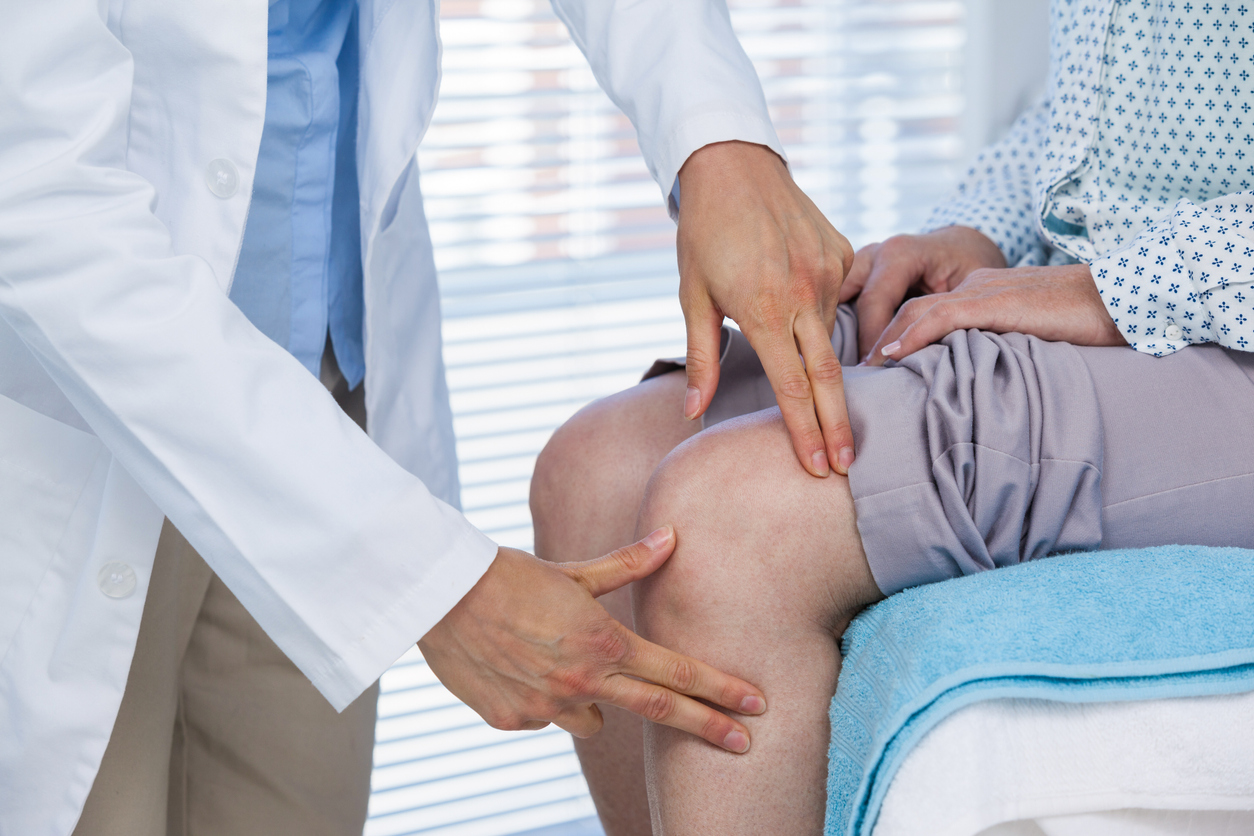
Diagnosing leg pain by medical professional
Diagnosing the cause of leg pain involves a comprehensive evaluation by a healthcare professional. Here are some steps typically involved in the diagnosis of leg pain:
The healthcare professional will start by gathering information about your medical history. They will inquire about the duration, location, and characteristics of the leg pain, as well as any associated symptoms or triggering events. They may also ask about your lifestyle, occupation, exercise habits, and any previous injuries or medical conditions that may be relevant.
A physical examination is conducted to assess the affected leg and identify any visible signs or abnormalities. The healthcare professional will inspect the leg for swelling, redness, warmth, or deformities. They may also evaluate the range of motion, strength, and sensation in the leg. Palpation and gentle pressure may be applied to specific areas to identify tender spots or areas of discomfort.
Based on the information gathered from the medical history and physical examination, further diagnostic tests may be ordered to help identify the cause of the leg pain. Common diagnostic tests include:
X-rays, ultrasound, CT scans, or MRI scans can provide detailed images of the bones, joints, muscles, and soft tissues in the leg. These tests help detect fractures, tumors, muscle tears, ligament damage, or other structural abnormalities.
Blood tests may be performed to evaluate for underlying medical conditions such as infections, autoimmune disorders, or metabolic abnormalities that could contribute to leg pain.
These tests assess the function of the nerves in the leg and can help diagnose conditions such as peripheral neuropathy or nerve compression.
The healthcare professional will consider a range of potential causes for the leg pain and perform a differential diagnosis to narrow down the possibilities. They will evaluate the symptoms, medical history, physical examination findings, and diagnostic test results to determine the most likely cause.
The first step is diagnosing the problem. PAD is often the sign of other even more serious underlying problems such as artery clogging around your heart and brain. These two issues can lead to heart attack and stroke, so you must not wait.
Doctors diagnose PAD using an ankle-brachial index, which is a painless test used to monitor blood flow through your arms and legs.
If the doctor notices that blood flows much better through your arms compared to your legs, they might move forwards with another noninvasive procedure such as a CTR or MRA to locate the blockage.
Leg pain of a vascular origin
Leg pain of vascular origin refers to pain in the legs that is caused by compromised blood flow due to vascular issues. It is primarily associated with peripheral arterial disease (PAD), a condition where the arteries that supply blood to the legs become narrowed or blocked by plaque buildup. The reduced blood flow to the legs leads to inadequate oxygen and nutrient supply to the muscles, resulting in pain and discomfort.
The pain experienced in the legs due to vascular problems is typically different from joint pain. It is often described as aching, cramping, or a feeling of heaviness in the muscles. Unlike joint pain, which tends to improve with activity, leg pain caused by vascular issues worsens with movement or exertion and stops when resting. This is because physical activity increases the demand for oxygen and nutrients in the muscles, which cannot be adequately met when there is restricted blood flow.
Other symptoms that may accompany leg pain of vascular origin include numbness, tingling, coldness, and weakness in the legs. Some individuals may also develop non-healing sores or wounds on the legs and feet, experience hair and nail changes, or notice changes in the skin color or temperature of the affected limb.
It is important to seek medical attention if you experience leg pain of vascular origin, as it may indicate an underlying vascular condition that requires diagnosis and treatment. Vascular specialists can perform diagnostic tests, such as the ankle-brachial index, Doppler ultrasound, or angiography, to assess blood flow and identify any blockages or abnormalities in the arteries.
Severe cases of leg pain and PAD
PAD, or peripheral arterial disease, can be related to gangrene, a serious condition that occurs when tissue dies due to a lack of blood supply. In PAD, the arteries that supply blood to the legs and feet become narrowed or blocked by plaque buildup, reducing blood flow to the affected areas. This restricted blood flow can deprive the tissues of oxygen and nutrients, leading to tissue damage and potentially gangrene.
When the blood supply is severely compromised in individuals with PAD, particularly in advanced stages of the disease, it can result in the development of non-healing wounds or ulcers on the legs or feet. These ulcers are more susceptible to infection, and if left untreated, the infection can progress and cause tissue death. In severe cases, gangrene can develop, leading to the decay and death of affected tissues.
Gangrene is a serious medical emergency that requires immediate treatment. It can lead to further complications, including the spread of infection, sepsis, and the potential need for amputation. Proper management of PAD, including lifestyle modifications, medication, and interventions like angioplasty or bypass surgery, can help improve blood flow, reduce the risk of tissue damage, and minimize the likelihood of developing gangrene. Regular monitoring and early intervention are crucial in preventing the progression of PAD to such severe complications.
When Is Vascular Treatment Required for Patients with Leg Pain?
The most significant sign of PAD is leg pain, which differs from joint pain. Understanding the difference is crucial because joint pain often improves with activity, while muscle pain related to PAD worsens with activity. In addition to muscle pain, other symptoms of PAD may include leg cramping, numb and cold feet or legs, slow-healing sores or wounds on the feet and legs, pale feet, pain in the feet worsened by leg elevation, poor nail and hair growth, and weakness in the legs. Most patients who develop this disease have a history of smoking. Recognizing these symptoms is important in determining when vascular treatment may be necessary for leg pain.
Common Causes of Leg Pain
Leg pain can result from various factors, including nerve, muscle, bone, and spine issues. However, it is essential to consider poor blood circulation as a potential cause of leg pain. Certain activities, such as walking or working, may exacerbate the pain, and it may subside when resting. Nighttime leg pain or leg cramping may indicate a severe form of PAD known as critical limb ischemia (CLI), where the pain persists throughout the night. Identifying the specific activities and patterns associated with leg pain can help in understanding the underlying vascular causes.
Think you may have vascular symptoms of leg pain?
Leg Pain Treatment: Step-by-Step Guide
Treating leg pain caused by vascular disease requires a comprehensive approach. The first step is proper diagnosis, which often involves tests such as the ankle-brachial index to assess blood flow in the arms and legs. Once diagnosed with PAD, lifestyle changes, including quitting smoking, adopting a healthier diet, and engaging in approved exercise, are recommended. Medication may also be prescribed to manage symptoms and prevent clotting. In some cases, minimally invasive treatments like angioplasty, stenting, or cryoplasty may be necessary to address blockages and improve blood flow. The ultimate goal of treatment is to alleviate leg pain, improve overall lifestyle, and prevent complications.
Medication for Leg Pain Treatment
The prognosis for leg pain treatment depends on early intervention and adherence to the prescribed treatment plan. Taking medication, such as low-dose aspirin, antiplatelet agents, or anticoagulants, can help thin the blood and prevent clotting. These medications are often prescribed and should be taken as directed by a healthcare professional. Prompt and appropriate treatment can lead to significant improvements in leg pain and reduce the risk of complications.
By understanding the signs of peripheral arterial disease (PAD) and the importance of seeking appropriate vascular treatment for leg pain, individuals can address underlying vascular issues and improve their overall quality of life. Consulting with a vascular specialist is crucial for accurate diagnosis, personalized treatment plans, and ongoing management of leg pain associated with vascular disease.
You can take some medications to help with symptoms of PAD; most of them require a prescription.
- Aspirin
Taking a low dose aspirin to thin out your blood is a known treatment for those at risk for heart disease. Do not take aspirin with any other blood thinners. - Antiplatelet Agents
Antiplatelet medications help prevent the blood from sticking together, which decreases your chances of developing a clot. - Anticoagulants
An anticoagulant will also help prevent a blood clot by thinning out the blood. - This can help keep blood flowing to your extremities even if you have narrow arteries due to plaque build-up.
What are the minimally invasive treatment options for leg pain caused by PAD?
Minimally invasive treatment options for leg pain caused by PAD (peripheral arterial disease) aim to improve blood flow to the affected areas and alleviate symptoms. These procedures are typically performed by vascular specialists and offer less risk, shorter recovery time, and reduced invasiveness compared to traditional surgery. Here are some common minimally invasive treatments for leg pain caused by PAD:

Angioplasty
This procedure involves inserting a thin catheter with a balloon on its tip into the blocked or narrowed artery. The balloon is inflated to widen the artery and improve blood flow. In some cases, a stent (a small mesh tube) may be inserted to keep the artery open.

Atherectomy
During an atherectomy, a special device is used to remove plaque buildup from the artery walls. This helps restore blood flow by clearing the blockage and creating a wider pathway for blood to pass through.
Arterial stent
In cases where the artery remains narrowed or prone to re-closing after angioplasty, a stent may be inserted. A stent is a small, mesh-like tube that acts as a scaffold to keep the artery open, maintaining improved blood flow.
These minimally invasive procedures can effectively relieve leg pain caused by PAD by restoring blood flow to the affected areas. The choice of treatment depends on the specific characteristics of the artery blockage and individual patient factors. A vascular specialist will evaluate the patient's condition and recommend the most appropriate treatment option to alleviate leg pain and improve overall vascular health.
Ready to speak with a vascular specialist?