Leading Chronic Venous Insufficiency Doctors
Chronic Venous Insufficiency (CVI) is a medical condition where the veins in your legs do not allow blood to flow back up to your heart efficiently. This occurs because the valves in the veins, which prevent the backward flow of blood, are damaged or weakened. As a result, blood can pool in the legs, leading to various symptoms and complications.
Chronic venous insufficiency (CVI) affects nearly half of the United States population to varying degrees, with a higher prevalence among individuals over 50 years old. Women are more frequently affected by factors such as pregnancy, which impacts blood flow to the legs.
What Are The Symptoms of Chronic Venous Insufficiency?
The severity of chronic venous insufficiency varies greatly depending on the progression of the disease. Your veins will not strengthen independently and will continue to weaken with time and age. With early intervention, you can avoid complications such as burst capillaries that change your skin color and problematic ulcers.
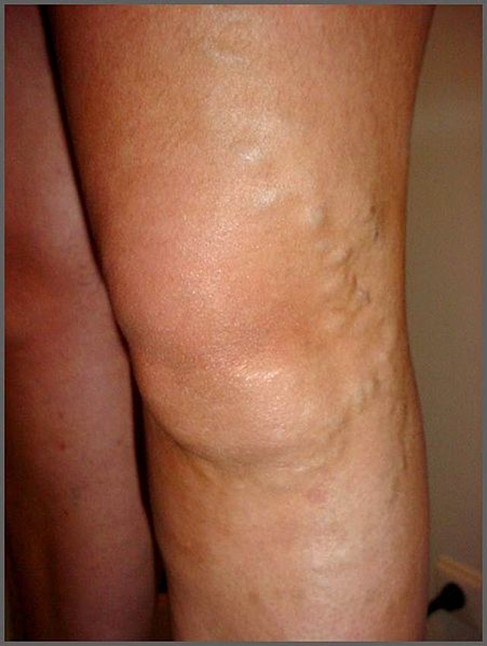
Photo Credit: Wikimedia Commons
The symptoms of CVI can vary in severity and may develop gradually. Here are the common symptoms associated with chronic venous insufficiency:
Swelling (Edema)
Swelling in the lower legs and ankles, particularly after long periods of standing or sitting.
The swelling may worsen throughout the day and improve after resting or elevating the legs.
Pain and Discomfort
Patients with chronic venous insufficiency can experience an aching, throbbing, or a feeling of heaviness in the legs. For many patients, the pain or discomfort in their legs may worsen with prolonged standing or sitting and improve with elevation or movement. Chronic venous insufficiency can also cause a feeling of heaviness, tiredness, or fatigue in the legs, especially after prolonged activity, which can be relieved by rest and leg elevation.
Ulcers and Skin Changes
Chronic venous insufficiency (CVI) results from prolonged high pressure in the leg veins, leading to chronic inflammation, tissue damage, and scar tissue. Symptoms include darkening or discoloration of the skin, dry and itchy skin, stasis ulcers, and leathery skin texture. These changes make the skin more prone to injury and can lead to venous ulcers or open sores, especially around the ankles. It can also cause thickened, hardened skin, known as lipodermatosclerosis, leading to itching and irritation.
Varicose Veins
For some patients, varicose veins can indicate chronic venous insufficiency (CVI). Veins have one-way valves that help blood flow toward the heart. In CVI, these valves can become weak or damaged, causing blood to flow backward (reflux) and accumulate in the leg veins. This can result in swollen, raised, blue, or purple twisted veins visible just under the skin. However, not all CVI patients will have varicose veins.
Leg Cramps and Restlessness
Reflux or venous return can lead to muscle cramps or spasms in the legs, especially at night. Additionally, individuals may experience restless leg syndrome, an uncontrollable urge to move the legs, and cramping and burning sensations.
When blood accumulates in the legs, it can reduce the delivery of oxygen and essential nutrients to the muscles. Muscles need a constant supply of oxygen to function correctly, and when this supply is reduced, it can result in muscle fatigue and cramps. Individuals with CVI may reduce their physical activity due to pain and discomfort, which can lead to muscle weakness and reduced physical condition.
Pitting Edema
Patients with chronic venous insufficiency may experience pitting edema. When pressure is applied to the swollen area, an indentation or "pit" remains for a few seconds, indicating fluid build-up in the surrounding tissues. Chronic Venous Insufficiency causes increased venous pressure, capillary leakage, and impaired lymphatic drainage, leading to fluid accumulation in the lower extremities.
Am I at Risk for Developing Chronic Venous Insufficiency?
Chronic Venous Insufficiency (CVI) does not have a single direct cause, but several factors can increase the likelihood of developing this condition. Those with a family history of vein problems, advancing age, or a history of multiple pregnancies are at higher risk for developing CVI.
Jobs that require long periods of sitting or standing, as well as obesity, can also contribute to CVI. Other known risk factors for developing chronic venous insufficiency include injuries or damage to the veins, a prior history of deep vein thrombosis (DVT), and even being tall. Understanding these risks can help take preventive measures and seek early treatment to manage CVI effectively.
Can I Prevent Chronic Venous Insufficiency?
If you are at high risk of developing chronic venous insufficiency (CVI) due to factors like obesity, smoking, or being over 50 years old, there are several steps you can take to mitigate this risk and improve your overall vascular health. Quitting smoking is crucial, as it improves overall vascular health. Losing excess weight, maintaining a healthy diet, and regular exercise can significantly reduce strain on your veins.
Avoid sitting or standing for prolonged periods; take breaks to move around if your job requires it. Adjust your workspace to relieve pressure on your legs, and consider wearing supportive shoes. While these actions can't wholly prevent CVI, they promote a healthy lifestyle and lower blood pressure, reducing the risk of venous insufficiency.
How is Chronic Venous Insufficiency Diagnosed?
At your appointment, your vascular specialist will obtain a detailed medical and vascular history, including medications you’re taking and any past surgeries or vascular treatments, and examine your legs for symptoms of chronic venous insufficiency.
Your Center for Vascular Medicine specialist might request venous duplex studies or ultrasound imaging to identify abnormal blood flow patterns in the legs' veins. This uncomplicated test provides the doctor with a visual representation of the leg veins' functionality. The images will indicate whether blood is flowing correctly or if deep vein thrombosis is present.
Other possible tests include various venograms, which insert a contrast into your veins to get quality images of potential blockages.
Treating Chronic Venous Insufficiency
Depending on how severe your chronic venous insufficiency (CVI) is, your doctor may suggest different treatment plans. In the early stages, the focus is on preventing painful swelling and ulcers. You can help by eating a healthy diet, exercising regularly, wearing compression socks, and changing positions often to improve blood flow. Your doctor might also prescribe medications to reduce your risk of blood clots.
To manage symptoms and slow the progression of CVI, consider using compression stockings, elevating your legs, exercising regularly, and maintaining a healthy weight. While these steps won't cure or reverse the condition, they can help you feel better and prevent it from worsening.
Depending on the severity of your chronic venous insufficiency, risk factors, and overall health, your vascular specialist may recommend one of several non-invasive procedures if other measures aren’t working or if symptoms such as severe ulcers or skin changes are not responding to treatment.
Minimally Invasive Procedures
The minimally invasive procedures for chronic venous insufficiency typically take about 1-2 hours. Most patients can return to normal activities on the same day with minimal restrictions. These treatments carry minimal risk, resulting in less bruising, and involve small incisions that cause minimal scarring. A vascular healthcare provider specializing in vein disease can help you determine what types of procedures, if any, would suit you. Center for Vascular Medicine offers more advanced treatments for patients who have not seen improvement in their symptoms after treatments like sclerotherapy or ablation.
Further assessments and treatments might be necessary for more severe vein problems, like post-thrombotic syndrome or iliac vein compression. These include venography, intravascular ultrasound (IVUS), venoplasty, and stent placement.
What Happens if Chronic Venous Insufficiency Goes Untreated?
If chronic venous insufficiency (CVI) goes untreated, it can progress from early signs like spider and varicose veins to more severe complications. Initially, you might notice excessive swelling in the calf and ankle area, accompanied by leg discoloration. Over time, untreated CVI can cause the skin to become thick and leathery.
In advanced stages, painful open ulcers may form on the skin, which are difficult to treat and can lead to severe infections.
Other complications include deep vein thrombosis, cellulitis, lipodermatosclerosis, lymphedema, stasis dermatitis, and superficial thrombophlebitis. Early treatment and management are essential to prevent these serious complications. It is crucial to consult a doctor when you notice spider or varicose veins to manage the condition early and prevent these severe complications.
Talk to your vascular specialist if you notice a change in your veins, an increasing number of spider or varicose veins, or symptoms of chronic venous insufficiency. Early detection and intervention are essential for patients struggling with chronic venous insufficiency.
Chronic Venous Insufficiency Treatment at Center for Vascular Medicine
If you notice symptoms like spider or varicose veins, leg swelling, or skin discoloration, it is essential to consult with a vascular specialist promptly. Early treatment options, including lifestyle changes, compression therapy, and minimally invasive procedures like ablation or sclerotherapy, can effectively manage symptoms and prevent the progression of CVI.
Untreated CVI can lead to severe complications, so timely medical attention is vital. Stay proactive about your vascular health and seek early intervention to maintain your quality of life and prevent serious issues.
Contact our vascular specialists to schedule a consultation and learn more about managing and preventing chronic venous insufficiency. Early detection and treatment are critical to a healthier, more comfortable life. Book an appointment or find a CVM location near you.
This article is a comprehensive overview of Chronic Venous Insufficiency. However, it should not take the place of speaking with a physician. If you are experiencing any of the symptoms listed above, or know someone who is, contact us today to schedule a consultation.
You can also view other vascular diseases below:

