Why Does My Period Hurt So Bad?
Many women experience pain and discomfort during their period. More than half of women say that they have pain for at least one day of every month due to menstruation. While painful periods are not uncommon, they are certainly uncomfortable.
There are two types of period pain: primary dysmenorrhea and secondary dysmenorrhea. Primary dysmenorrhea involves pain that usually starts with your very first period. Many women find that their period pain diminishes as they get older. Women who have given birth often find that their pain is less after that.
Secondary dysmenorrhea does not begin with your first period–it tends to occur later in life. Many women with secondary dysmenorrhea find that it gets worse over time; this type of pain is usually caused by a reproductive disorder.
Why Do Period Cramps Hurt?
If you find yourself asking, “Why does my period hurt so bad?” it can be helpful to understand the cause of the pain. There are compounds in the body called prostaglandins that are structurally similar to a fat molecule but functionally more like a hormone. These compounds cause the uterus to contract and shed its lining every month–this is why you feel cramps.
We will take the example of a patient pseudo named Jane who had recurring pain a year after the birth of her second child. Jane started having the pain every month, and the pain would last from a few days to a week. Many doctors she visited dismissed her pain, with one saying he wouldn't treat her any longer. This is her story.
Back Pain and Period Pain
Prostaglandins can also be the cause of back pain during menstruation. If you have higher levels of these compounds, your pain is likely to be more intense. Some women experience pain and discomfort in their legs during menstruation as well. Back pain can also be caused by conditions such as endometriosis, fibroids, or pelvic inflammatory disease.
Pregnancy brings enormous musculoskeletal, physiological, and emotional changes to a woman’s body. Along with these changes, they also experience back pain due to physiological and musculoskeletal changes. It is one of the common problems that women suffer due to the postural changes of pregnancy, increased ligamentous laxity, and decreased abdominal muscle function.
Jane's symptoms emerged a year after the birth of her child. The pain was located in her lower abdomen, and it would switch between a heavy ache and a sharp pain. Many other causes must be ruled out like acid reflux and appendicitis. She was sure that it was not acid reflux but was prescribed antacid relief medication.
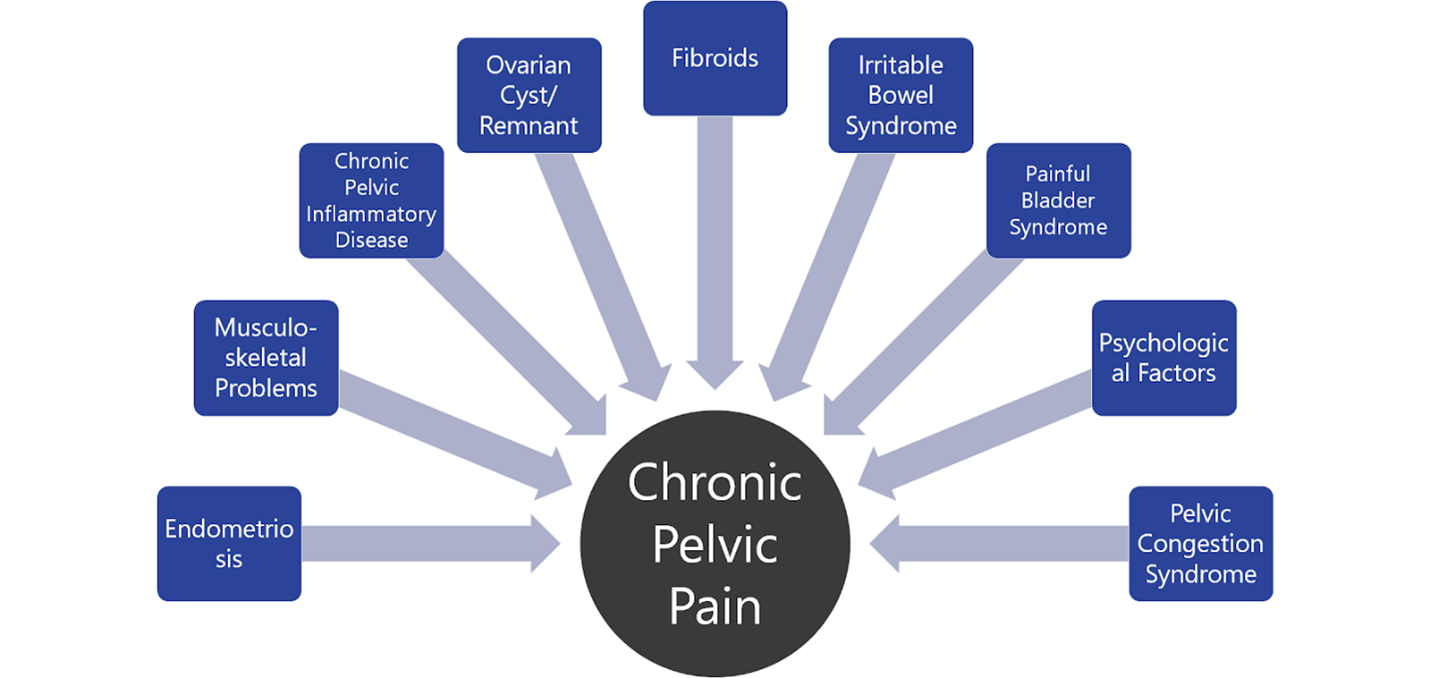
Finding Possible Causes of Pelvic Pain
While many women experience pain during their period due to normal cramping, there are other possible reasons for pain.
Ovarian Cysts
Ovarian cysts often go unnoticed and do not cause any pain or discomfort. However, cysts can also cause pelvic and lower abdominal pain. Bloating, vomiting, and fever are all signs of ovarian cysts as well. If a cyst ruptures, this can cause severe pain and bleeding and requires immediate medical attention.
Endometriosis
Endometriosis is a disorder that can cause pelvic pain, back pain, and heavy bleeding. Other symptoms of endometriosis include diarrhea, nausea, fatigue, and pain during sex. Infertility is also associated with this disorder.
Fibroids
Uterine fibroids are benign growths in the uterus that often don’t cause pain or discomfort. Depending on the location of the fibroids, and if they are large or multiple, they can cause pelvic and back pain as well as heavy bleeding. Other signs of fibroids include constipation and frequent urination.
Intrauterine Device (IUD)
Using an IUD for birth control can also cause pain similar to menstrual cramps. Some women don’t experience any symptoms when they use an IUD, while others just feel cramping and discomfort while it is being inserted. After insertion, some women experience cramping and heavy bleeding for up to six months. This is more common with copper IUDs.
Pelvic Inflammatory Disease
Pelvic pain can be the result of pelvic inflammatory disease which results from an infection in the reproductive system. This disease can affect the ovaries, uterus, or fallopian tubes. Signs of pelvic inflammatory disease include frequent and painful urination, pain during sex, unusual vaginal discharge, lower abdominal, and pelvic pain, and fever.
In the case of Jane, she was recommended to undergo endometrial ablation, which is a procedure typically used when a patient has heavy periods. She had severe periods and felt like sleeping all day along with her major bloating and abdomen pain. Fearing that it might not benefit her case, and seeing the potential side effects, she canceled the endometrial ablation procedure.
When to See an OBGYN After Period Period Cramps?
It can be difficult to know what is normal period pain and what is cause for concern. It is always best to err on the side of caution and see your healthcare provider if you feel something isn’t right. Here are some indications that a visit to your OBGYN might be required.
Other Symptoms Accompany Pain
If you are experiencing additional symptoms along with menstrual cramping, this can be a sign that something more serious is going on. Symptoms such as dizziness, nausea, and vomiting, or fever are not typically associated with menstruation.
Heavy or Irregular Bleeding
A significant increase in the amount of bleeding during your period can be cause for concern. While every woman’s flow is different, excessive bleeding can be both a symptom and a cause of other problems. Bleeding that occurs outside of the span of your menstrual period is also an indication that you should speak to a healthcare provider.
Interference with Daily Activities
Most women have occasionally experienced period pain that causes them to miss a day of work or school. However, if the pain is regularly interfering with your ability to fulfill your daily responsibilities, this is a sign that you should make an appointment with your OBGYN.
Cramping for a Prolonged Time Period
It is normal to experience cramps at the beginning of your period, for a day or two. Some women also have cramps the day before menstruation starts. Cramping that lasts for your whole period or continues after your period ends is unusual.
Unexplained Pain
Women who experience painful periods generally only have pain during the first few days of menstruation. Some women will also have discomfort during ovulation. However, if you are experiencing pelvic pain outside of these times, you should see a health care provider. Another indication that something else may be occurring is if you have pain during sex.
Pain Medications Not Effective
Taking medication such as ibuprofen or acetaminophen when you have cramping is generally helpful for most women. If you find that these medications do not provide relief of your pain, make an appointment to see your OBGYN.
In Jane’s case, she started feeling pain in her back as well. When she visited her rheumatologist, her blood work came back normal. At that point Jane couldn’t handle another negative test and needed an answer. Her primary care doctor ordered a urinalysis and an ultrasound scan of Jane’s abdomen and pelvis.
The urinalysis found blood in Jane’s urine, and the ultrasound completed by a vascular specialist finally unveiled the cause of Jane's pain: she had Pelvic Congestion Syndrome.
Pelvic congestion syndrome occurs when blood pools in the pelvis. It often emerges during or after pregnancy where the veins become engorged and cause blood to pool. That pooling can lead to severe pain, especially when standing or standing for an extended period of time. The development of varicose veins around the ovaries is a common symptom of pelvic congestion syndrome.
Jane was successfully treated with a venogram procedure and a venous stent was placed to open the vein and allow for proper blood drainage.
When to see a vascular doctor?
Debilitating pain associated with periods could be a sign of an underlying health condition.
The example used above regarding heavy/excessive bleeding could be symptoms of anemia and would require an evaluation.
Feeling generally unwell is also something that heavy menstrual bleeding can cause, including feeling tired, dizzy, short of breath and sometimes causing poor memory.
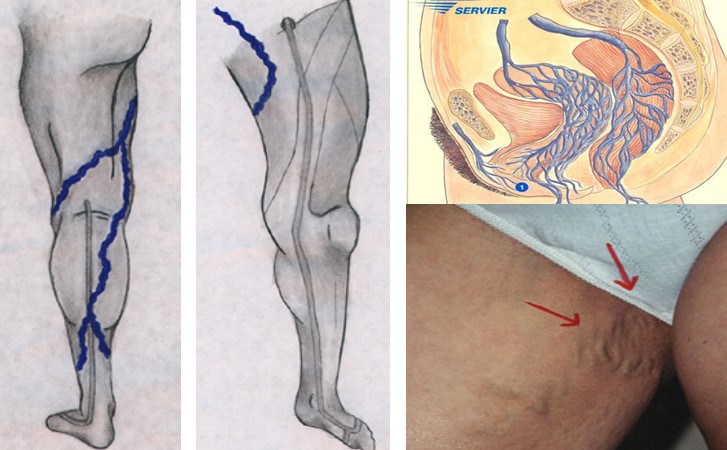
Patients who suffer from painful and heavy periods could be at risk of varicose veins in their pelvic area. Many people are familiar with enlarged, bulging and dark purple veins on their legs, but experts have now warned that similar veins can also be present in the lower abdomen.
The varicose veins could be a sign of Pelvic Congestion Syndrome (PCS). This is created when increased blood pressure blows out the valves in the veins. Pelvic Congestion Syndrome is a vascular disorder affecting the veins of the pelvic region because there is not proper drainage of blood out of the region.
This is a painful condition and symptoms can be mistaken for a range of issues such as constipation, diarrhea, endometriosis, cyst, and fibroids as we saw in Jane’s case. A vascular specialist can make a correct diagnosis using ultrasound, looking at your history, and performing a detailed physical.
Final Thoughts on Period Pain
Cramping a day or two before your period, and the first couple of days during menstruation is normal and experienced by many women. Pain that occurs outside of these times, pain that is severe, or pain that is accompanied by other symptoms should be evaluated.
Women know themselves best and should trust their instincts if something doesn’t feel right. If you suspect that there is something more going on than just period cramps, make an appointment with your healthcare provider. When pelvic symptoms last for 6 months or longer and the patient has visited a gynecologist, then it is best to get an evaluation from a vascular doctor to see the proper blood flow of the veins in the pelvic region. The non-invasive evaluation is completed by a trained specialist.

