Venous Hypertension or Venous Insufficiency: What Is the Difference?
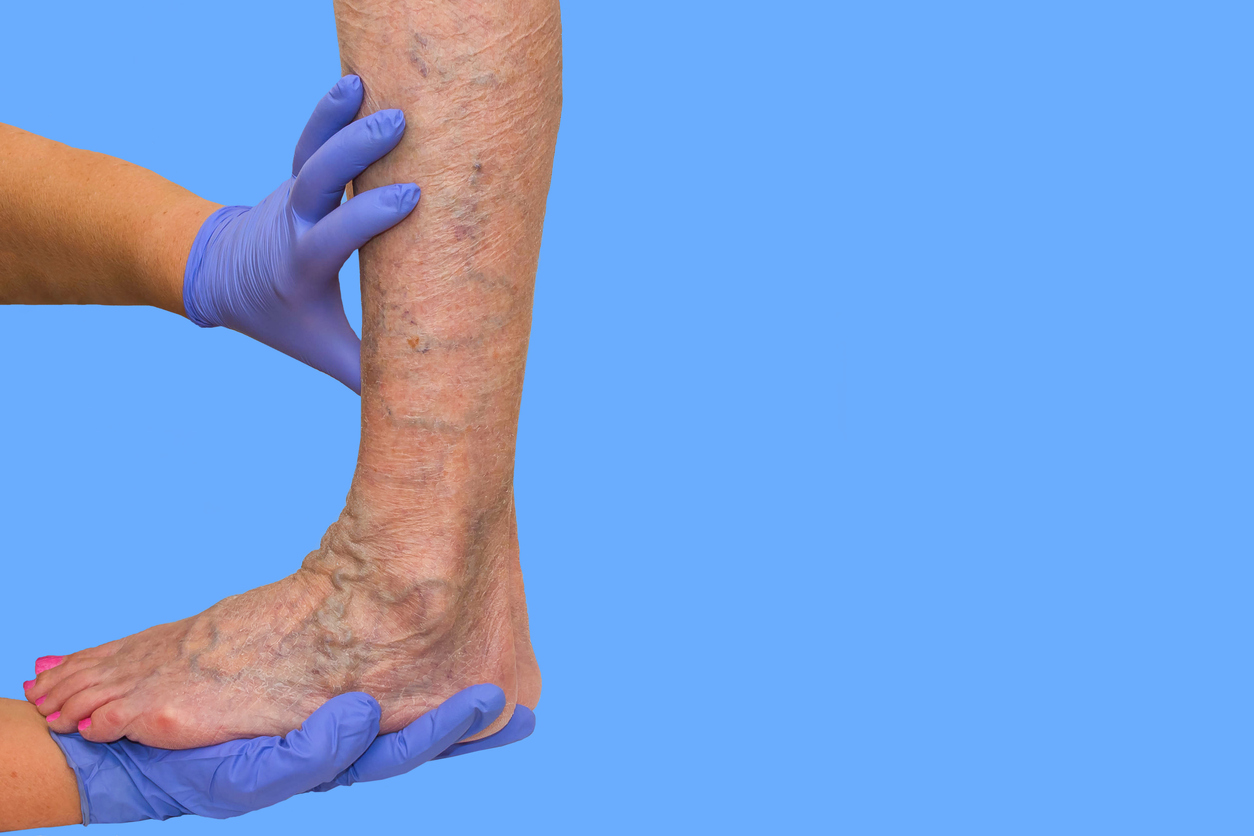
Several venous pathologies can have serious complications. Chronic venous insufficiency (CVI) is an umbrella term containing multiple venous diseases. Venous insufficiency can refer to chronic venous reflux disease and chronic venous hypertension.
Venous Insufficiency
Venous Insufficiency is a chronic condition characterized by compromised blood flow from the legs to the heart. A pilot study reveals that chronic venous pathology is highly prevalent. It typically coexists with cardiovascular diseases and other comorbidities.
In cases of venous insufficiency, the damaged veins in the legs cannot deliver the right volume of blood back to the heart, leading to blood pooling in the legs. Multiple underlying pathologies can result in insufficiency.
Venous Hypertension: A Complication of Venous Insufficiency
Venous hypertension is one of the conditions that might arise due to venous insufficiency. Microvascular venous hypertension is a prominent feature of chronic venous disease. As stated, the incompetent valves of the veins in CVI lead to the pooling of blood in the legs.
This pooled blood can significantly increase the blood pressure in the leg veins. Studies reveal that venous hypertension is associated with chronic venous disease and can alter the endothelial surfaces of the veins.
Causes
The most common causes of CVI are listed below.
Family History
A majority of individuals suffer from CVI due to familial traits. A family history of varicose veins and deep venous thrombosis can contribute to CVI. People with venous insufficiency in family members are more prone to developing the disorder.
Deep Venous Thrombosis
DVT, or deep venous thrombosis, is the name given to a condition in which blood clots form inside the deep veins of the leg, damaging a valve. Therefore, DVT is a common cause of venous insufficiency. Thrombosis in calf veins can hinder the normal function of the vessels.
Varicose Veins
Swollen, enlarged, and twisted superficial veins (especially in the legs) are called varicose veins. The abnormal veins are common in patients with lower extremity venous insufficiency. Studies show that varicose veins are a prominent risk factor for deep vein thrombosis. Around 2/3rd of DVT patients have a co-existing venous disease (chronic).
Muscle Weakness
The propulsion of blood in the veins depends on the movement of muscles in the extremities. Disorders that weaken the leg muscles can also contribute to venous insufficiency. Compromised calf muscle activity (due to immobility or abnormal gait) can lead to venous hypertension and CVI.
Risk Factors
Specific risk factors are identified for venous insufficiency and hypertension. The most common ones are as follows:
Age and Gender
CVI can affect any gender, but the disorder is more common in older women than men. Pregnant and post-menopausal women are at greater risk of CVI.
Obesity
Being obese or overweight significantly increases your chances of acquiring venous insufficiency and hypertension. Research suggests that old males having a high BMI are more prone to falling prey to CVI.
Pregnancy
The pregnancy period is marked by hemodynamic changes and increased venous pressure (venous hypertension). The rise in venous blood pressure is attributed to hormonal abruptions and changes in smooth muscle activity. The increased pressure and reduced flow rate during pregnancy predispose expecting mothers to develop venous insufficiency.
Smoking/Tobacco Use
A case-control study highlighted the link between smoking and venous insufficiency. It is believed that tobacco consumption increases the oxidative stress of the body (by promoting carbon monoxide and nitric oxide levels). That can explain the association between lower limb venous insufficiency and cigarette smoking.
Symptoms
Symptoms of CVI are below.
Leg Pain
Almost all patients suffering from CVI experience leg pain. There is a lack of studies correlating the extent of pain with the severity of the disease. Conservative treatment strategies are frequently adopted to manage this pain.
According to a 2020 study, fatigue, discomfort, and pain are the most noticeable symptoms of chronic venous hypertension. These symptoms significantly reduce the quality of life.
Pain increases on movement. However, it is noted that people who habitually do light walking have milder symptoms.
Edema of the Legs (Swelling)
The lack of blood clearance from the lower extremity veins and the increased pressure inside induce fluid leaking into the soft tissues. This pooling of interstitial fluid is a common feature of CVI and is known as edema. Significant pitting edema is associated with CVI and venous hypertension.
Leg Cramps
Venous insufficiency patients often have trouble sleeping due to nocturnal leg cramps. Muscular cramps are also common in venous insufficiency patients.
Leg Ulcers
Hindrances in the blood flow promote the formation of leg ulcers. Thus, the treatment of CVD promotes ulcer healing in patients. A venous leg ulcer is a debilitating complication of a complex vascular disease.
Skin Pigmentation
Some patients notice a change in the color of their legs. Skin pigmentation is most prominent in the ankle region. Excessive deposition of melanin and hemosiderin pigment is the root cause of skin pigmentation in venous hypertension patients. More levels of pigmentation are seen in the advanced stages of the disease.
Chronic Venous Insufficiency Treatment
CVI and venous hypertension treatment aims to reduce edema and improve the blood flow in the veins. The most effective treatment strategies for venous hypertension include:
Compression and Elevation
Applying external pressure on the legs can reduce the edema and promote blood flow back to the heart. Different types of stockings are designed to apply sufficient pressure on the legs. Compression stockings and wraps are good at reducing lymphedema.
Textile-based compression interventions are now used for managing leg edema and hypertension.
Keeping the legs elevated can be beneficial in managing CVI-induced leg ulcers and reducing pressure in the leg veins. People suffering from the disease due to prolonged standing can obtain relief from symptoms by elevating the leg.
Exercise
Light, regular exercise is linked to evident improvements in venous insufficiency symptoms. Exercise training can improve calf muscle function, ultimately reducing venous hypertension in the legs. Different exercise strategies promote wound healing and can be used as adjuvants to treat CVI.
Medicines
Your doctor will also advise you to take diuretic medicines to drain the extra fluids accumulated in the body. Anticoagulants are an essential part of the regimen. These drugs act as blood thinners and prevent the clotting of the blood. Pentoxifylline is also given to improve blood flow.
Surgery
Surgical interventions are reserved for severe cases of venous insufficiency and hypertension. Endoscopic surgeries are prevalent because they are minimally invasive procedures. Laser treatment and surgical repair of the valves are also effective options for CVI and venous hypertension.

