Top Sign of Peripheral Artery Disease (PAD): Hole in Between Toes
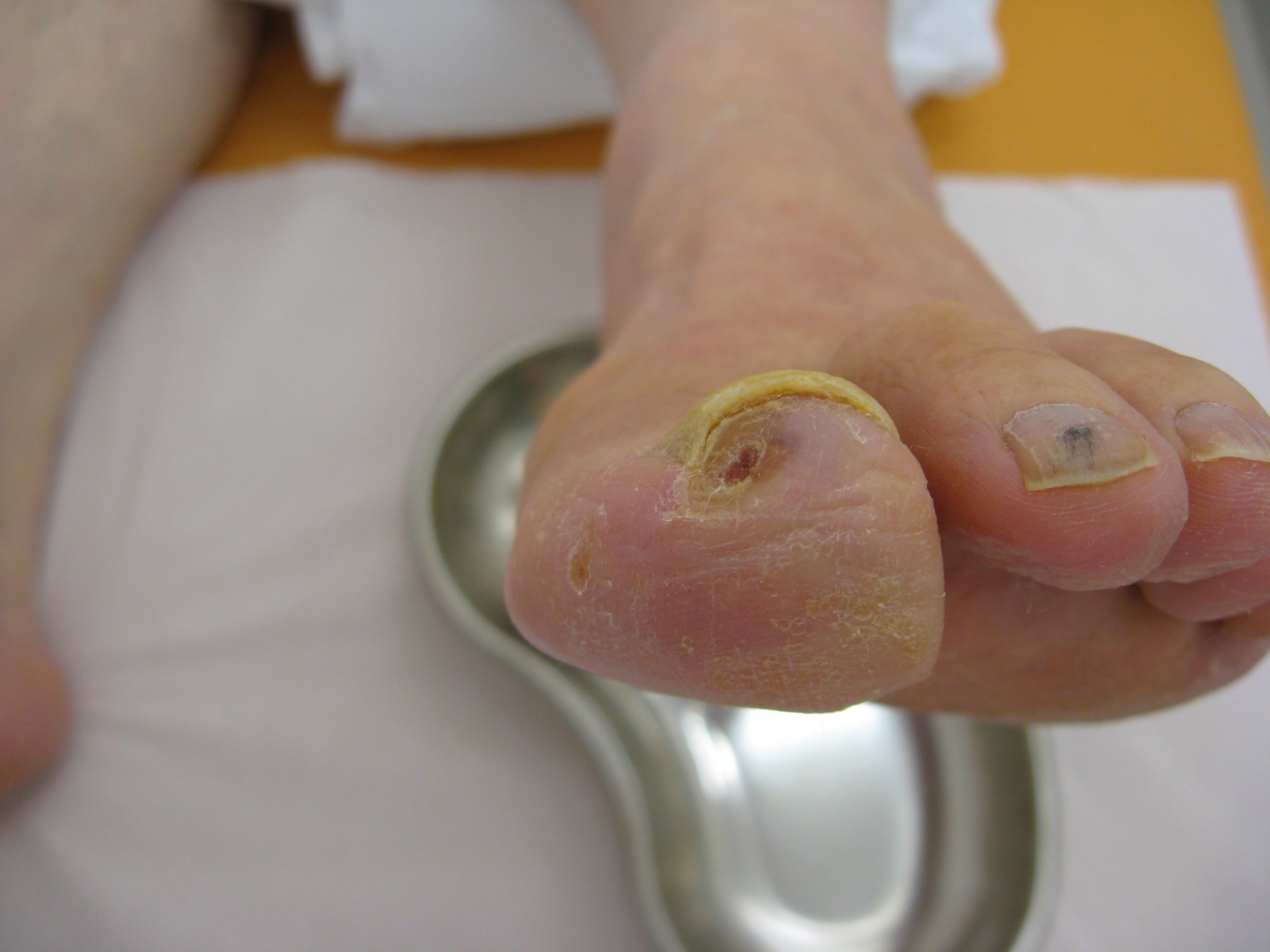
Peripheral Artery Disease (PAD) is a circulatory condition, which refers to the blockage of blood vessels that carry blood to the lower extremities. It often goes unnoticed and undiagnosed, due to symptoms that closely mimic other health conditions – like arthritis.
However, awareness about the more distinct signs of PAD, such as a hole in between toes, can clearly demonstrate PAD pathogenesis and help in detection and treatment.
Understanding PAD
Peripheral Artery Disease is characterized by narrowed arteries reducing blood flow to the limbs, primarily affecting the legs and feet.
The primary cause of PAD is atherosclerosis, a condition where plaque, consisting of fat, cholesterol, and fibrin, accumulates on the inner walls of the arteries. This build-up narrows the arteries, decreasing or blocking blood flow.
While PAD can manifest with symptoms like leg pain while walking (claudication), numbness or weakness in the leg, or even coldness in the lower leg or foot, some people with PAD do not experience any overt symptoms.
That's where unusual signs, such as a non-healing wound or hole in between toes, can serve as significant indicators of PAD.
When there's a reduced blood flow to the extremities due to PAD, even a small wound or cut can take an unusually long time to heal. As time progresses, these wounds can deepen into a hole that extends to underlying tissues, a condition known as foot ulceration. These ulcers most commonly occur in pressure points of the foot, such as in between toes, and their healing is further impaired due to inadequate blood supply.
Ignoring such a sign can have serious implications as the site is susceptible to infections, eventually leading to gangrene and necessitating amputation in severe cases.
When Should a Patient Visit a Vascular Surgeon?
A patient should consider visiting a vascular surgeon for a hole in the bottom of the foot when the wound is not healing or shows signs of infection, particularly if they have risk factors or symptoms related to poor blood circulation. Vascular surgeons specialize in treating conditions that affect the blood vessels and can play a crucial role in the management of foot wounds, especially when there are concerns about blood flow to the affected area.
Here are some indications that warrant a visit to a vascular surgeon for a hole in the bottom of the foot:
Lack of Healing - If the hole or wound on the foot has not shown signs of improvement or healing despite proper wound care and treatment, it may indicate underlying circulation issues that require assessment.
Signs of Infection - Redness, warmth, swelling, increased pain, foul-smelling discharge, or fever may indicate that the wound has become infected. Infected wounds can be particularly concerning, especially if there are underlying vascular problems, as they can lead to serious complications.
Presence of Peripheral Artery Disease (PAD) - Patients with a history of peripheral artery disease, characterized by reduced blood flow to the legs and feet, may experience delayed wound healing or have an increased risk of non-healing wounds.
Peripheral Neuropathy - Individuals with peripheral neuropathy (nerve damage) associated with conditions like diabetes may not have normal sensation in their feet, making them more susceptible to injuries and unaware of developing wounds.
Pain or Discomfort in the Leg or Foot - Pain or cramping in the calf or foot, especially during walking (intermittent claudication), could indicate compromised blood flow that may affect wound healing.
History of Vascular Disease - Patients with a history of vascular conditions, such as deep vein thrombosis (DVT) or previous vascular surgeries, should be vigilant about foot wounds and consider evaluation by a vascular surgeon if necessary.
Non-Healing Ulcers in Multiple Locations - If a patient has experienced multiple non-healing ulcers on different areas of the foot, it could indicate an underlying vascular issue that requires further investigation.
It's crucial to seek medical attention promptly for any foot wounds that are not healing or appear infected, especially if you have diabetes or other risk factors for vascular disease. A vascular surgeon can assess the blood flow to the foot, identify any underlying issues, and develop a comprehensive treatment plan to promote proper wound healing and prevent complications.
Treatment for PAD
The primary goal of PAD treatment is to manage the symptoms, stop the progression of atherosclerosis, and lower the risk of complications.
Treatment generally involves permanent lifestyle modifications, medications, and in some cases, surgical intervention.
Lifestyle modifications form the cornerstone of PAD treatment. This includes adopting healthy diets, low in saturated fat and cholesterol. It also incorporates regular physical activity, quitting smoking, and managing related conditions – like diabetes and hypertension. These health conditions are known risk factors for atherosclerosis and PAD.
Medications may be prescribed to control symptoms, prevent the formation of blood clots, lower blood pressure, reduce cholesterol levels, and manage pain. Antiplatelet agents like aspirin or clopidogrel, cholesterol-lowering drugs such as statins, antihypertensives, and cilostazol to relieve leg pain are commonly prescribed.
In severe cases, or when symptoms do not improve with conservative treatment, surgical procedures may be recommended.
This could involve angioplasty, where a small balloon is used to widen the narrowed or blocked artery, often followed by placing a small metal tube called a stent to keep the artery open. In other cases, bypass surgery may create a new route for blood flow around the blocked artery.
Early detection and timely treatment of PAD can significantly improve quality of life and prevent complications. Therefore, a hole in between the toes as a potential sign of PAD is a key precursor to diagnosis. It's always advisable to consult with a healthcare provider if you notice any of the aforementioned warning signs.
